What You Need to Know About Medicare Premiums 2026
Medicare premiums 2026 are increasing significantly, with the standard Part B premium rising to $202.90 per month—a nearly 10% jump from 2025. If you’re approaching retirement or already enrolled in Medicare, understanding these changes is essential to avoid surprises in your budget.
Quick 2026 Medicare Premium Summary:
| Medicare Part | Cost Type | 2026 Amount | Change from 2025 |
|---|---|---|---|
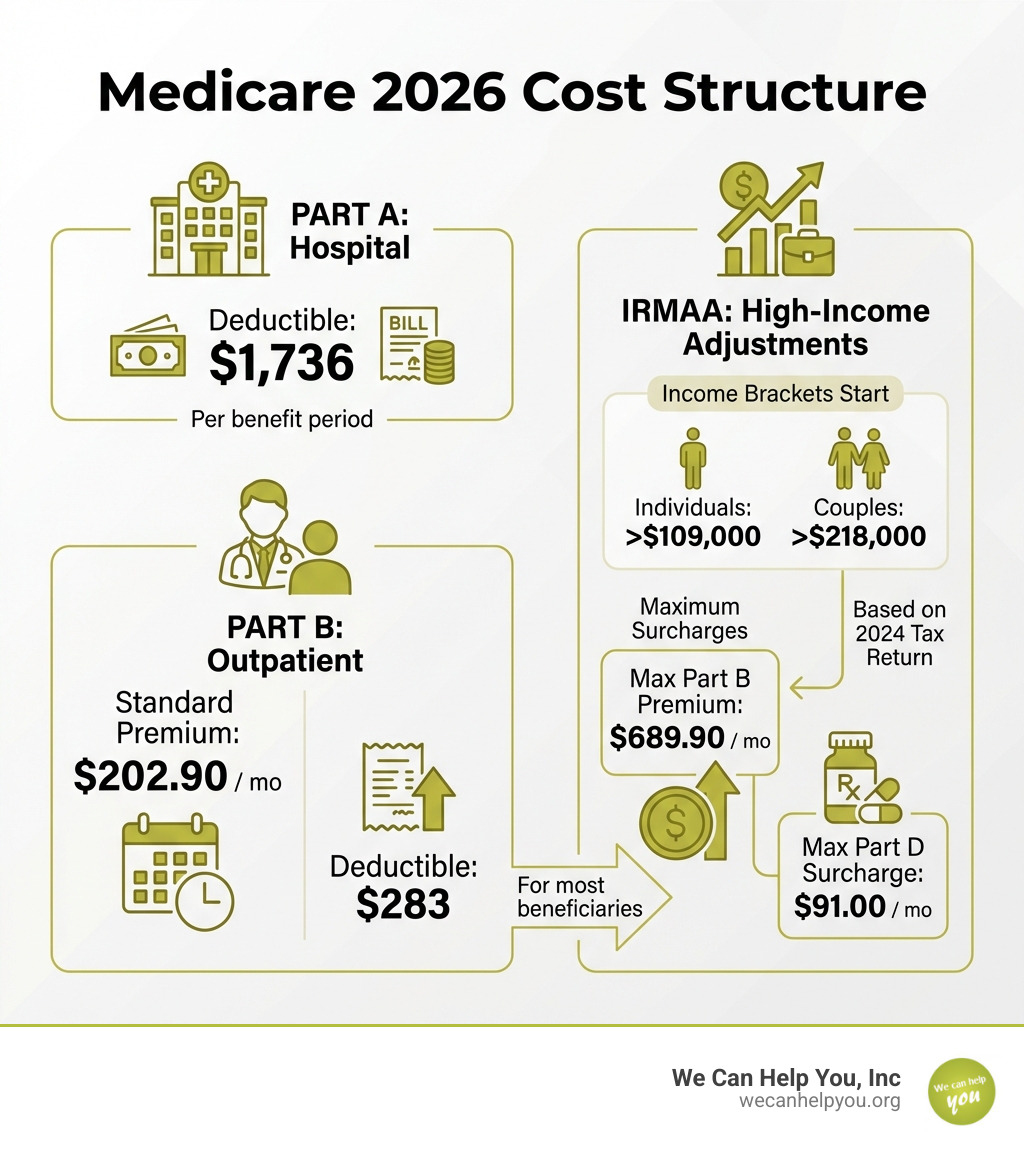
| Part B | Standard Premium | $202.90/month | +$17.90 (9.7%) |
| Part B | Annual Deductible | $283 | +$26 |
| Part B | High-Income Premium (IRMAA) | $284.10 – $689.90/month | Varies by income |
| Part A | Hospital Deductible | $1,736 per benefit period | +$60 |
| Part D | Income Adjustment (IRMAA) | $14.50 – $91.00/month | Added to plan premium |
Key facts you should know:
- About 8% of Medicare beneficiaries pay higher premiums due to income-related adjustments (IRMAA)
- The Part B premium increase will consume over 25% of the 2.8% Social Security cost-of-living adjustment
- 99% of beneficiaries qualify for premium-free Part A if they paid Medicare taxes while working
- Income from your 2024 tax return determines whether you’ll pay IRMAA surcharges in 2026
These cost increases mean Medicare will take a bigger bite out of your Social Security check or retirement income. The Part B premium alone will exceed $2,400 annually for most enrollees, and high-income beneficiaries could pay more than $8,200 per year just for Part B coverage.
Understanding exactly what you’ll pay—and why—helps you plan your retirement budget accurately and avoid costly mistakes.
Understanding Medicare Premiums 2026: Part B and Beyond
When we talk about Medicare costs, Part B often takes center stage because it is the portion of the program most beneficiaries pay for directly out of their monthly budget. Medicare Part B covers your “outpatient” care—think doctor visits, preventive screenings, and durable medical equipment.
For 2026, the Centers for Medicare & Medicaid Services (CMS) has calculated the rates based on the projected costs of providing these services. This calculation involves determining the “actuarial rate,” which represents the average monthly cost of the program per person. By law, the standard Medicare Part B Premium is set to cover approximately 25% of the total expected cost of the program for aged enrollees, with the federal government’s general fund covering the remaining 75%.
According to Official CMS 2026 Part B data, the monthly actuarial rate for aged enrollees in 2026 is $405.40. While that sounds like a lot of math (and it is!), the result is a standard premium that feels quite heavy for many retirees. We know that navigating these numbers can feel like trying to read a map in a thunderstorm, but being prepared is the best way to keep your retirement plan on track.

Standard Medicare Premiums 2026 and Deductibles
The headline for the year is the $202.90 standard monthly premium. This is an increase of $17.90 from the 2025 rate of $185.00. While a 9.7% increase might not sound like a world-ending shift, it marks the first time the base premium has crossed the $200 threshold. For a couple both on Medicare, this means an annual cost of over $4,800 just for Part B premiums alone.
In addition to the premium, we have the annual deductible. The 2026 Medicare Part B Premiums announcement also confirmed that the annual deductible will rise to $283. This is a $26 increase from the $257 deductible in 2025. You must pay this amount out-of-pocket for covered services before Medicare begins to pay its share (typically 80% for most services).
It is interesting to note that the 2026 premium includes a small $0.20 repayment amount. This is the final year of a multi-year effort to repay the U.S. Treasury for prior balances related to legislative changes in 2015 and 2021. Once 2026 concludes, that specific debt will be settled.
Immunosuppressive Drug Coverage Only
A specialized category of Medicare exists for individuals who have had a kidney transplant. Normally, Medicare eligibility based on End-Stage Renal Disease (ESRD) ends 36 months after a successful transplant. However, many of these individuals still need expensive immunosuppressive drugs to keep their new kidney healthy.
Thanks to the Consolidated Appropriations Act details, there is a Part B “immunosuppressive drug only” benefit. For 2026, the standard premium for this specific coverage is $121.60. This is significantly lower than the full Part B premium because it only covers those specific medications and not the full range of outpatient services. It provides a vital safety net for those who might otherwise lose access to life-saving medication after their transplant-related Medicare expires.
High-Income Adjustments: How IRMAA Impacts Medicare Premiums 2026
If you have a higher income, you might find that your medicare premiums 2026 are significantly higher than the standard $202.90. This is due to the Income-Related Monthly Adjustment Amount, or IRMAA. We often describe IRMAA as a “surcharge” for those who have been financially successful in their later years.
The Social Security Administration (SSA) determines who pays IRMAA by looking at your Modified Adjusted Gross Income (MAGI) from your tax return from two years prior. So, for your 2026 premiums, the SSA will look at your 2024 tax return. Understanding Medicare IRMAA Charges is crucial because these surcharges are not optional; they are added directly to your Part B and Part D premiums.
Approximately 8% of all Medicare beneficiaries are subject to 2026 IRMAA adjustments. If your income has dropped significantly since 2024 due to a “life-changing event” (like retirement or the death of a spouse), you can appeal this determination, but otherwise, the brackets are strictly enforced.
Part B IRMAA Tiers for 2026
The IRMAA brackets for 2026 start for individuals with a MAGI above $109,000 and married couples filing jointly with a MAGI above $218,000. As your income moves into higher tiers, the percentage of the program costs you are responsible for increases from 25% up to 85%.
For 2026, the Part B monthly premiums including IRMAA are:
- Individual $109,001 – $137,000 (Joint $218,001 – $274,000): $284.10 total
- Individual $137,001 – $171,000 (Joint $274,001 – $342,000): $405.80 total
- Individual $171,001 – $205,000 (Joint $342,001 – $410,000): $527.50 total
- Individual $205,001 – $499,999 (Joint $410,001 – $749,999): $649.30 total
- Individual $500,000+ (Joint $750,000+): $689.90 total
If you are in the highest bracket, you are paying nearly $700 a month per person for Part B! This is why many of our clients ask, Is it Possible to Reduce My Medicare Part B Premium? While you can’t “negotiate” with the government, strategic financial planning—such as managing RMDs or using tax-efficient withdrawal strategies—can sometimes help you stay below a specific threshold.
Part D Income-Related Adjustments
IRMAA doesn’t stop at Part B; it also applies to Part D (prescription drug coverage). Unlike Part B, where everyone pays the same base premium to the government, Part D premiums vary based on the private insurance plan you choose. However, the IRMAA surcharge is a fixed amount paid directly to Medicare, regardless of which plan you have.
For 2026, the Part D IRMAA surcharges range from $14.50 to $91.00 per month. These amounts are calculated using the 2026 national base beneficiary premium of $38.99. Even if you have a Part D plan with a $0 premium (common in some Medicare Advantage plans), you must still pay the IRMAA surcharge if your income exceeds the thresholds. Medicare IRMAA Charges can add over $1,000 a year to your drug coverage costs in the highest bracket.
Medicare Part A and Hospitalization Costs
While Part B covers your doctors, Medicare Part A covers the big stuff: inpatient hospital stays, skilled nursing facility care, and some home health services. Most people think of Part A as “free,” but that isn’t entirely accurate. While the premium might be $0 for most, the out-of-pocket costs when you actually use the hospital can be substantial.
According to the Medicare.gov cost overview, Medicare Part A uses “benefit periods.” A benefit period begins the day you are admitted to the hospital and ends when you haven’t received any inpatient care for 60 days in a row. This means you could potentially pay the Part A deductible multiple times in a single year if you have multiple hospitalizations spaced apart.
Premium-Free Part A Eligibility
We have good news here: approximately 99% of Medicare beneficiaries do not pay a monthly premium for Part A. This is because you (or your spouse) likely paid Medicare taxes for at least 40 quarters (10 years) while working. If you meet this requirement, you’ve already “pre-paid” your Part A premiums through your working years.
If you don’t meet the 40-quarter requirement, you aren’t left out in the cold, but you will have to “buy in” to the program. Understanding these Medicare Costs is vital for those who immigrated to the U.S. later in life or spent many years in the home without paying into the Social Security system.
Costs for Part A Buy-In and Coinsurance
For those who must pay a premium for Part A in 2026, the rates have increased:
- Full Premium: $565 per month (for those with fewer than 30 quarters of coverage). This is a $47 increase from 2025.
- Reduced Premium: $311 per month (for those with 30-39 quarters of coverage). This is a $26 increase from 2025.
Even if your premium is $0, you still face the 2026 Medicare Costs associated with hospital stays. The Part A inpatient hospital deductible will be $1,736 in 2026, an increase of $60 from 2025.
Once you are in the hospital, Medicare covers the first 60 days in full after you pay that deductible. If your stay lasts longer, you’ll face daily coinsurance:
- Days 61-90: $434 per day (up from $419 in 2025).
- Days 91 and beyond (Lifetime Reserve Days): $868 per day (up from $838 in 2025).
- Skilled Nursing Facility (Days 21-100): $217 per day (up from $209.50 in 2025).
Comparing 2025 vs. 2026 Medicare Costs
When we look at the transition from 2025 to 2026, the trend is clear: healthcare is getting more expensive. The nearly 10% increase in Part B premiums is particularly striking when compared to the 2.8% Social Security cost-of-living adjustment (COLA).
For many retired workers, the Part B premium will reach an all-time high of 9.4% of their average Social Security benefit. In simple terms, the “raise” you get from Social Security is being eaten up by the “bill” from Medicare. In fact, the premium hike will consume more than a quarter of the average COLA increase.
You might be wondering, Will My Medicare Premiums Rise in 2026? For the vast majority of the 65 million enrollees, the answer is yes. The total premium increase across the entire population is estimated to be $14.0 billion.
The Impact of the Hold-Harmless Provision
There is a silver lining for some beneficiaries called the “hold-harmless” provision. This law is designed to prevent your net Social Security check from decreasing from one year to the next due to Part B premium increases.
If the increase in your Part B premium is greater than the dollar amount of your Social Security COLA, the government will typically cap your premium increase so that your monthly check stays the same. However, this protection usually only applies to people who have their premiums deducted directly from their Social Security checks and who do not pay IRMAA. As we Prepare for Tomorrow: What to Expect for 2027 Medicare Costs, it’s important to keep an eye on how these protections interact with inflation.
Frequently Asked Questions about Medicare Premiums 2026
What is the difference between a premium and a deductible?
Think of a premium like your monthly Netflix subscription—it’s what you pay every month just to have the coverage active. A deductible is more like the “cover charge” at a club—it’s the amount you have to pay out-of-pocket for services before the insurance company (or Medicare) starts picking up the tab. Paying for Medicare Premiums is a recurring monthly task, while the deductible is usually an annual hurdle.
How does my 2024 income affect my 2026 Medicare costs?
Medicare uses a “two-year lookback” period. The Social Security Administration receives data from the IRS to determine your IRMAA status. Because tax returns are filed in the year after the income is earned, the most recent verified data available for 2026 is from the 2024 tax year. Understanding Medicare IRMAA Charges and How to File an Appeal is vital if your income has since dropped, as you don’t want to be penalized for money you are no longer making.
What are the coinsurance rates for Part A in 2026?
As mentioned earlier, Part A coinsurance kicks in during long hospital stays. In 2026, you’ll pay $434 per day for hospital days 61 through 90. If you stay longer than 90 days, you begin using your 60 “lifetime reserve days,” which cost $868 per day. For those in a skilled nursing facility, the first 20 days are covered at 100%, but days 21 through 100 will cost you $217 per day. These Medicare Premiums and coinsurance amounts represent a significant financial risk if you don’t have supplemental insurance like Medigap.
Conclusion
Navigating medicare premiums 2026 can feel overwhelming, but you don’t have to do it alone. At We Can Help You, Inc., our mission as a non-profit is to provide the education you need to make informed decisions about your retirement. Whether you are in Florida, New York, Texas, or any of the states we serve, we are dedicated to helping you protect your financial future.
We offer a free Medicare Planning Guide and a free Social Security maximization report to help you find ways to increase your retirement income and offset these rising costs. Don’t let the 2026 price hikes catch you off guard. Start your 2026 Medicare planning today and ensure your golden years stay bright.



