The Medicare Eligibility Disability Waiting Period Explained
The medicare eligibility disability waiting period is a mandatory 24-month window that most people receiving Social Security Disability Insurance (SSDI) must wait before their Medicare coverage begins.
Here’s the quick answer:
| Stage | Timeframe |
|---|---|
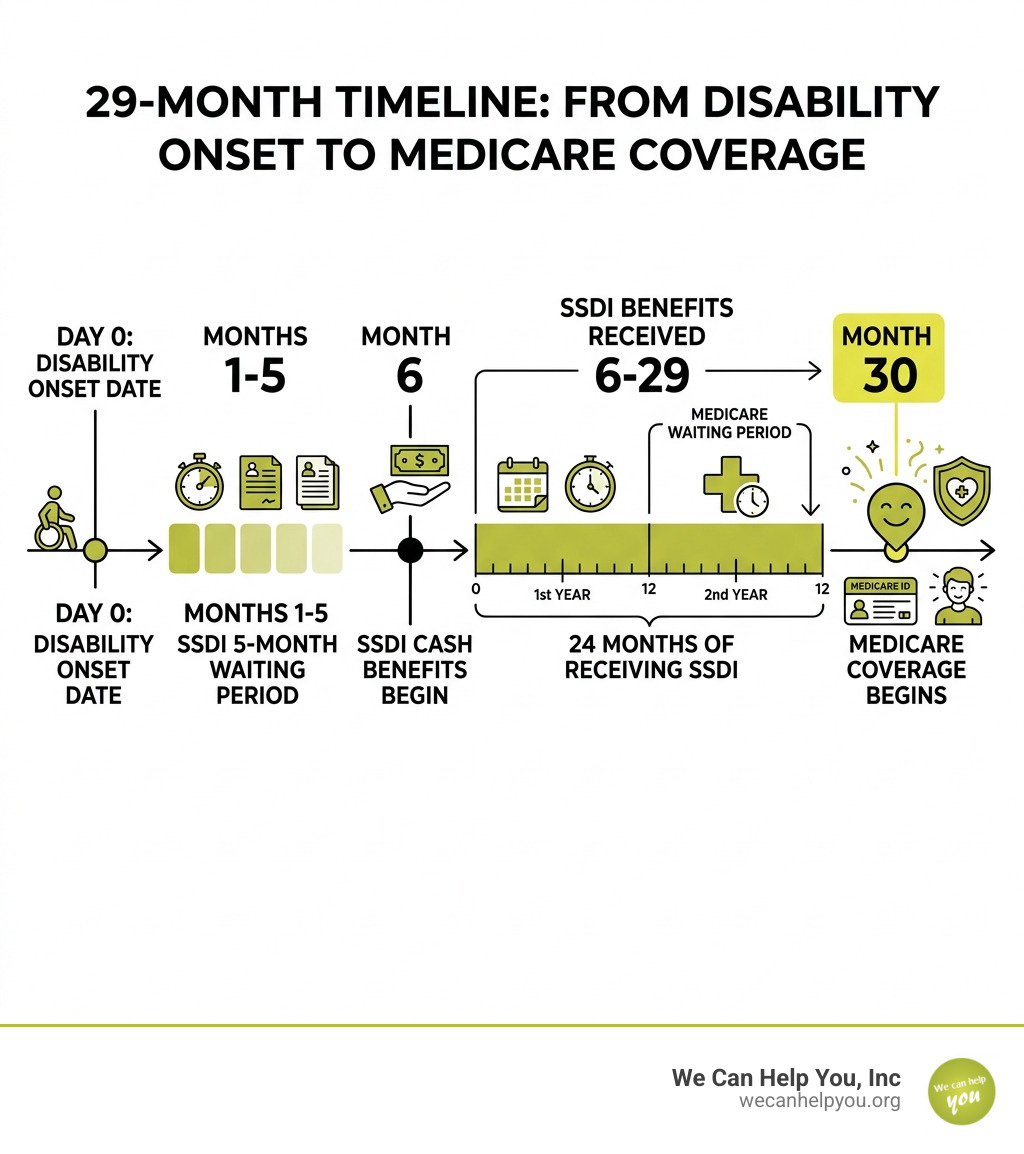
| Disability onset date | Day 0 |
| SSDI 5-month waiting period | Months 1-5 |
| SSDI cash benefits begin | Month 6 |
| Medicare waiting period | 24 months of receiving SSDI |
| Medicare coverage begins | Month 25 of SSDI benefits (~Month 30 from onset) |
| Exceptions | ALS: immediate; ESRD: as early as month 4 of dialysis |
So in practice, from the moment you become disabled to the day Medicare kicks in, you could be waiting close to 29 months total.
That’s a long time to go without coverage — especially when you’re already too sick to work.
When Congress expanded Medicare to people with disabilities back in 1972, it built in this delay on purpose. The goal was to control costs and make sure benefits went to those with serious, long-lasting conditions. But for the roughly 1.8 million people caught in this gap today, the wait is anything but abstract. Nearly 4% of people die before their Medicare coverage ever starts.
If you’re navigating SSDI and trying to figure out when your health coverage begins — and what to do in the meantime — this guide walks you through everything you need to know.
Understanding the Medicare Eligibility Disability Waiting Period

To understand why this gap exists, we have to look back at the Social Security Amendments of 1972. Before this time, Medicare was strictly for those aged 65 and older. When Congress decided to expand the program to include people with significant disabilities, they were worried about two things: cost and “crowding out” private insurance.
Lawmakers wanted to ensure that Medicare didn’t accidentally replace private group health plans that people might still have through a spouse or a previous employer. They also wanted to be absolutely certain that a disability was “severe and long-lasting” before the government took over the tab for healthcare. By creating a 24-month wait, they effectively created a “test of time” to confirm the disability was permanent.
While this helped with cost containment for the federal budget, it created a massive hurdle for the individual. According to the Medicare Two-Year Waiting Period Fact Sheet, nearly 39% of people in this waiting period find themselves without any health insurance at some point, and 24% have no coverage for the entire duration of the wait.
Calculating Your Medicare Eligibility Disability Waiting Period
Calculating exactly when your coverage starts can feel like a high-stakes math problem. It all starts with your “Established Onset Date” (EOD)—the date the Social Security Administration (SSA) decides your disability actually began.
Once your EOD is set, the clock starts. However, you don’t actually start the 24-month Medicare clock until you have finished a separate 5-month waiting period for SSDI cash benefits. This means you are eligible for Medicare in the month after you have received 24 months of SSDI checks. In most cases, this makes the total wait 29 months from the day you became disabled.
If you are confused about the difference between these various “clocks,” you can read more info on waiting periods vs elimination periods to see how these timelines interact in insurance.
Automatic Enrollment for Disability Beneficiaries
The good news is that once you’ve cleared the 24-month hurdle, you don’t usually have to fill out a mountain of paperwork to get your basic coverage. The SSA automatically notifies the Centers for Medicare & Medicaid Services (CMS) when you hit your 25th month of SSDI entitlement.
About three months before your coverage is set to begin, you should receive an enrollment package in the mail. This package includes your red, white, and blue Medicare card. You will be automatically enrolled in:
- Medicare Part A (Hospital Insurance): This is usually premium-free for SSDI recipients because you paid into the system through your payroll taxes while working.
- Medicare Part B (Medical Insurance): This covers doctor visits and outpatient care. Unlike Part A, Part B has a monthly premium that is typically deducted directly from your SSDI check.
If you already have Part A and only need to apply for Part B online, you can do so through the SSA website, though most disability beneficiaries are handled automatically.
The 5-Month SSDI Wait vs. the 24-Month Medicare Wait
It is a common misconception that the 5-month SSDI wait and the 24-month Medicare wait run at the same time. They actually run consecutively.
- The 5-Month SSDI Wait: When you are approved for disability, the SSA does not pay you for the first five full calendar months of your disability. Your “entitlement” to cash benefits begins in the sixth month.
- The 24-Month Medicare Wait: The Medicare clock only starts ticking once you are entitled to those cash benefits.
Because the SSDI approval process can take a long time (sometimes years), you might receive a large “retroactive” payment for back-dated cash benefits. If your retroactive payment covers 24 months or more of past benefits, you might actually qualify for Medicare immediately upon approval! You can find more technical details on this in the Medicare Information for Disability Research archives.
Critical Exceptions: When the Wait is Waived
There are two specific health conditions where the government recognizes that a 24-month wait is simply not feasible. For these conditions, the standard medicare eligibility disability waiting period is either shortened or eliminated entirely.
The two main exceptions are:
- ALS (Amyotrophic Lateral Sclerosis): Also known as Lou Gehrig’s disease.
- ESRD (End-Stage Renal Disease): Permanent kidney failure requiring dialysis or a transplant.
You can read the official Medicare coverage of kidney dialysis and transplant services guide for a deep dive into how these exceptions work.
Immediate Coverage for ALS Patients
For individuals diagnosed with ALS, the law is much more compassionate. Because ALS is a rapidly progressive and terminal condition, Congress removed the 24-month waiting period for Medicare in 2001. Later, in 2020, they also removed the 5-month waiting period for SSDI cash benefits for ALS patients.
If you have ALS, your Medicare coverage begins the very first month you are eligible for SSDI benefits. There is no two-year wait. You can learn more about the specifics of this waiver at the ALS Medicare waiting period waiver resource page.
Medicare Eligibility Disability Waiting Period for ESRD
If you have ESRD, your Medicare eligibility is not tied to SSDI benefits in the same way. Instead, it is tied to your treatment schedule. Generally, Medicare coverage for ESRD begins on the first day of the fourth month of your dialysis treatments.
However, you can get coverage even faster (starting the first month of dialysis) if you participate in a self-dialysis training program at a Medicare-approved facility to learn how to administer your own treatments at home. Medicare can also cover you retroactively for ESRD; if you wait a few months to apply, they can backdate your coverage to when your dialysis first hit that 4-month mark. Check out the End-Stage Renal Disease basics for more on this.
Bridging the Gap: Coverage Options During the Wait
If you don’t have ALS or ESRD, you have to find a way to pay for healthcare during those 24 months. This is often the most stressful part of the disability process. It’s important to know when to enroll in Medicare so you don’t miss your window, but what about the time before that?
Here are the most common ways we help people bridge the gap:
- COBRA: If you recently left a job with 20 or more employees, you can keep your employer’s insurance for up to 18 months (and sometimes up to 29 months if you are disabled). The downside? You usually have to pay 102% of the total premium, which can be incredibly expensive.
- Medicaid: If your income and assets are very low, you may qualify for Medicaid. In many states, being approved for SSDI makes you “categorically needy,” helping you get coverage while you wait for Medicare.
- The Marketplace (ACA): You can buy a private plan through Healthcare.gov. Because you are no longer working, you may qualify for significant premium tax credits that make these plans much more affordable than COBRA.
Managing Costs During the Medicare Eligibility Disability Waiting Period
Going uninsured during the wait is dangerous. Statistics show that previously uninsured individuals who finally enroll in Medicare require 20% more hospital visits and have medical expenditures 1.87 times higher than those who had coverage. Essentially, forgoing care during the 24-month wait makes you sicker and more expensive to treat later.
If you miss your initial window to sign up for Medicare because you were holding onto other coverage, you need to know how to sign up for Medicare without penalties. Missing the window can lead to a lifetime 10% surcharge on your Part B premiums for every year you waited.
Working While Disabled and Medicare Coordination
Many people worry that if they try to return to work, they will lose their Medicare. Fortunately, the SSA has “Work Incentives” to prevent this.
- Trial Work Period (TWP): You can work and earn any amount for up to 9 months (within a 5-year window) without losing your SSDI or Medicare. You can check the current Trial Work Period thresholds to see how much you can earn before a month counts toward your TWP.
- Extended Period of Medicare Eligibility: Even if you earn enough to stop your SSDI cash benefits, you can usually keep your premium-free Medicare Part A for at least 93 months (7 years and 9 months) after your trial work period ends.
If you are working and have an employer group health plan, who pays first?
- Small Employers (<100 employees): Medicare is usually the primary payer.
- Large Employers (100+ employees): The employer plan is primary, and Medicare is secondary.
Frequently Asked Questions about Medicare Disability
Can I decline Medicare Part B during the waiting period?
Yes, you can decline Part B, but we usually advise against it unless you have “creditable” coverage (like a plan from a current employer with over 100 employees). If you decline Part B and don’t have other coverage, you will face late enrollment penalties later and may have to wait for the General Enrollment Period (January–March) to sign up again, leaving you with no coverage in the meantime. To decline, you typically use Form CMS-1763, but talk to a counselor before doing so.
How does Medicare coordinate with VA or TRICARE benefits?
If you have both Medicare and VA benefits, they don’t actually “coordinate” in the traditional sense. You generally have to choose which system to use. The VA only pays for care at VA facilities or for VA-authorized “Community Care.” Medicare pays for care at civilian hospitals.
For TRICARE, once you are eligible for Medicare, you must enroll in Part B to keep your TRICARE coverage (which then becomes TRICARE For Life). You can find more on TRICARE and Medicare coordination at their official site.
What happens to my disability Medicare when I turn 65?
When you turn 65, your Medicare status “flips” from disability-based to age-based. This is actually a great thing! It gives you a “second chance” Initial Enrollment Period. If you had a Part B penalty from your disability years, it disappears. You also get a fresh 6-month window to buy a Medigap (Medicare Supplement) policy without medical underwriting—something that is often very difficult or expensive for disabled people under 65.
If you are approaching this milestone, you should ask yourself, “Do I need to enroll in Medicare at 65?” to ensure you don’t miss this one-time opportunity to reset your coverage.
Conclusion
The medicare eligibility disability waiting period is one of the most challenging aspects of the American healthcare system. Waiting two years for coverage while dealing with a life-altering disability is a burden no one should carry alone.
At We Can Help You, Inc., we are dedicated to educating people in states like New York, Florida, Texas, and across the country on how to navigate these complex rules. Whether you are in Albuquerque, NM, or Charlotte, NC, our mission is to provide you with the tools you need for a secure future.
We offer a free Medicare Planning Guide and a free Social Security maximization report to help you understand your benefits and increase your retirement income. Don’t let the waiting period leave you in the dark. Start your Medicare planning today and let us help you bridge the gap to the coverage you deserve.



