Why Medicare Enrollment Dates Matter
Medicare enrollment periods explained can feel overwhelming, but understanding when you can sign up or change your coverage is essential to avoid costly penalties and ensure you have the health insurance you need.
Once you know your key dates, you can act at the right time instead of scrambling later. Missing an enrollment window can lead to:
- Late enrollment penalties that can last as long as you have Medicare
- Gaps in coverage that leave you without important health insurance protection
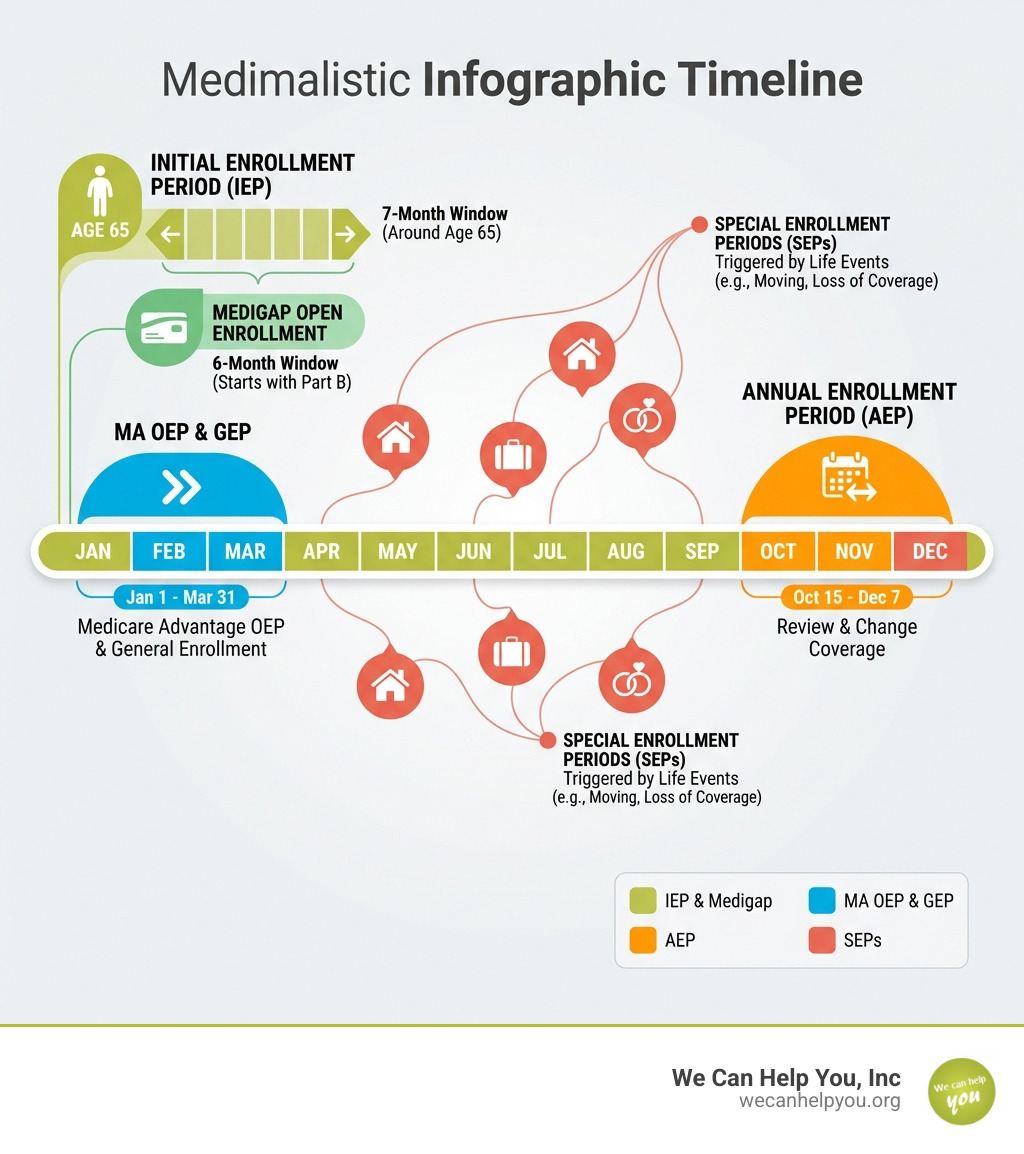
Here are the main Medicare enrollment periods you need to know:
- Initial Enrollment Period (IEP): A 7-month window around your 65th birthday when you first become eligible for Medicare
- Annual Enrollment Period (AEP): October 15 – December 7 each year, when you can review and change your Medicare coverage
- Medicare Advantage Open Enrollment Period (MA OEP): January 1 – March 31, for those already in a Medicare Advantage plan
- General Enrollment Period (GEP): January 1 – March 31, if you missed your Initial Enrollment Period
- Special Enrollment Periods (SEPs): Time-limited windows triggered by qualifying life events like moving or losing other coverage
- Medigap Open Enrollment Period: A 6-month window starting when you turn 65 and enroll in Part B
Once you understand these periods and mark them on your calendar, navigating Medicare enrollment becomes much simpler. The rest of this guide briefly explains each enrollment period, when coverage starts, and how to avoid common mistakes.
Your First Chance: The Initial Enrollment Period (IEP)
Congratulations, you’re approaching a new chapter, and for many, that means Medicare eligibility. Your very first opportunity to enroll in Medicare is during your Initial Enrollment Period (IEP). This is a 7-month window that sets the stage for your Medicare journey.
For most people, the IEP is a 7-month period that includes the three months before you turn 65, your birthday month, and the three months after. For example, if your 65th birthday is in June, your IEP would run from March 1st to September 30th.
If you’re under 65 and have received Social Security or Railroad Retirement Board disability benefits for 24 months, your IEP will start 21 months into your disability and last through the 28th month. There are exceptions for certain conditions like ALS and End-Stage Renal Disease (ESRD), where the 24-month waiting period for disability benefits is waived.
During your IEP, you can sign up for:
- Original Medicare (Part A and Part B): Part A is hospital insurance, and Part B is medical insurance.
- Medicare Advantage (Part C): An all-in-one alternative to Original Medicare offered by private companies. Many plans include prescription drug coverage and extra benefits.
- Medicare Part D (Prescription Drug Coverage): If you choose Original Medicare, you can add a stand-alone Part D plan for your medications. Medicare Advantage plans often include Part D.
Automatic Enrollment: If you’re already receiving Social Security or Railroad Retirement Board benefits at least four months before your 65th birthday, you’ll generally be automatically enrolled in Original Medicare (Part A and Part B). Otherwise, you’ll need to actively sign up.
Coverage Start Dates During Your IEP:
- If you enroll in the three months before your birthday month: Your coverage will typically start on the first day of your birthday month.
- If you enroll during your birthday month: Your coverage will start the month after you enroll.
- If you enroll in the three months after your birthday month: Your coverage will be delayed, starting two or three months after you enroll.
Understanding these timelines is crucial to avoid any gaps in your health coverage. For more details on this, we recommend checking out When does Medicare coverage start? and When Do You Need to Enroll in Medicare?.
The Main Medicare Enrollment Periods Explained
Once you’re enrolled in Medicare, there are several other important periods throughout the year when you can make changes to your coverage.
The Annual Enrollment Period (AEP): Your Yearly Review
The Annual Enrollment Period (AEP) runs from October 15 to December 7 each year. During this time, all current Medicare beneficiaries can review existing coverage and make changes for the upcoming year.
During AEP, you can:
- Switch from Original Medicare to a Medicare Advantage plan (Part C)
- Switch from a Medicare Advantage plan back to Original Medicare
- Join, change, or drop a Medicare Part D prescription drug plan
- Switch Medicare Advantage plans (with or without drug coverage)
Even if you’re happy with your current plan, review your Annual Notice of Change (ANOC), which explains next year’s costs and benefits. Changes made during AEP take effect on January 1st of the following year. For more tips, see What to Do During the Medicare Annual Enrollment Period.
The Medicare Advantage Open Enrollment Period (MA OEP)
If you’re in a Medicare Advantage plan and find it’s not the right fit, the Medicare Advantage Open Enrollment Period (MA OEP) runs from January 1 to March 31 each year.
During the MA OEP (if you are already in a Medicare Advantage plan), you can:
- Switch to a different Medicare Advantage plan (with or without drug coverage)
- Drop your Medicare Advantage plan and return to Original Medicare, and, if you wish, add a stand-alone Medicare Part D plan
This period is not for switching from Original Medicare to Medicare Advantage. Changes become effective the first day of the month after your new plan receives your enrollment request. Learn more in What to Do During the Medicare Advantage Open Enrollment Period.
The General Enrollment Period (GEP): A Second Chance for Parts A & B
If you missed your Initial Enrollment Period (IEP) and do not qualify for a Special Enrollment Period, the General Enrollment Period (GEP) is your fallback chance to sign up for Medicare Part A and/or Part B.
The GEP runs from January 1 to March 31 each year.
Using the GEP can mean:
- Delayed coverage (your coverage begins after you enroll, rather than right away at 65)
- Late enrollment penalties for Part B (and possibly Part A) if you did not have other creditable coverage
If you’ve missed your initial window, it is important to act during the GEP. To understand more about what to do, see Missed Medicare at 65? What to Do Next.
The Medigap Open Enrollment Period: A Critical Window
Medicare Supplement Insurance (Medigap) policies help pay for out-of-pocket costs not covered by Original Medicare, like deductibles, copayments, and coinsurance.
The best time to buy a Medigap policy is during your Medigap Open Enrollment Period. This is a six-month window that starts the first day of the month you turn 65 and are enrolled in Medicare Part B.
Why this period matters:
- Insurance companies cannot use medical underwriting during this window
- You have guaranteed issue rights to buy any Medigap policy sold in your state, regardless of health
If you miss this 6-month window, you might have to answer health questions, pay higher premiums, or be denied coverage. For more, see More about guaranteed issue rights and Is a Medigap Plan Right for You?.
When Life Changes: Understanding Special Enrollment Periods (SEPs)
Life events can change your health coverage needs, and sometimes you cannot wait for the next Annual Enrollment Period. That is where Special Enrollment Periods (SEPs) come in.

SEPs allow you to make certain changes to your Medicare coverage outside the standard enrollment periods due to specific qualifying life events. These periods are limited in duration, typically lasting for 2 to 3 months.
Qualifying Life Events for Medicare Advantage and Part D SEPs
Most SEPs for Medicare Advantage and Medicare Part D allow you to join, switch, or drop a plan when events such as these occur:
- Moving: You move outside your plan’s service area or into an area with new plan options
- Losing Other Coverage: You lose other creditable health coverage, such as employer-sponsored coverage or COBRA
- Plan Contract Changes: Your Medicare plan leaves Medicare, or Medicare ends its contract with your plan
- Qualifying for Extra Help: You qualify for Extra Help (Low-Income Subsidy) to pay for prescription drug costs
- Institutionalization: You move into, live in, or move out of a facility like a nursing home or skilled nursing facility
- Exceptional Conditions: Events such as being released from incarceration, being affected by a natural disaster, or receiving incorrect information from a federal entity
- 5-Star Plan Availability: A one-time SEP lets you switch to a Medicare Advantage or Part D plan rated 5 stars, available between December 8th and November 30th
SEP length varies by situation, but many last up to two full months after the event.
You can find a more complete list of qualifying events and their rules at find a complete list of qualifying events here. If your move is the reason for your SEP, our article on Medicare Special Election Change of Residence might be helpful.
How Special Enrollment Periods for Original Medicare (Parts A & B) work
SEPs also apply to Original Medicare (Parts A and B), especially if you worked past 65 and had employer-sponsored health coverage.
If you delayed signing up for Medicare Part B (and premium Part A, if applicable) because you or your spouse (or family member if disabled) were actively working and covered by an employer group health plan, you may avoid the Part B late enrollment penalty.
Once that employer coverage or the employment ends, you qualify for an 8-month Special Enrollment Period to sign up for Part A and/or Part B. This 8-month SEP starts the month after your employment ends or your group health plan coverage ends, whichever comes first.
Some coverage types, such as COBRA or retiree coverage, generally are not considered “group health plan coverage” for avoiding the Part B late enrollment penalty. In those cases, you usually need to enroll during your IEP or another valid SEP to avoid penalties.
To apply for Part B during this SEP, you typically need proof of your employer coverage, often using forms like CMS-40B and CMS-L564. If you have Part A and want to sign up for Part B, you can Apply Online If you already have Part A, go to SSA.gov to sign up for Part B.Apply OnlineYou can also send completed forms toyour local Social Security office by fax or mail.Download forms:I want to sign up for Part A and Part BI have Part A and want to sign up for Part B.
For more guidance on coordinating Medicare with employer coverage, see Working Past 65: Do You Need Medicare Part B If You Have Employer Insurance?.
The Cost of Waiting: Penalties and Coverage Gaps
Understanding Medicare enrollment periods helps you avoid significant financial consequences. Missing your enrollment windows can lead to lifelong late enrollment penalties and gaps in coverage.
Understanding Medicare Late Enrollment Penalties
If you do not sign up when you are first eligible and do not qualify for a Special Enrollment Period, you may pay more for coverage.
- Part B Penalty: Your monthly premium may increase by 10% for each full 12-month period you could have had Part B but did not sign up. You pay this penalty for as long as you have Part B.
- Part D Penalty: If you go without creditable prescription drug coverage for 63 consecutive days or more after your Initial Enrollment Period ends, you will likely pay a penalty. Medicare calculates this by multiplying 1% of the national base beneficiary premium by the number of full months you went without Part D or creditable coverage. This amount is added to your Part D premium for as long as you have Part D.
- Premium-Part A Penalty: If you must pay a Part A premium and do not buy it when first eligible, your premium may go up by 10%. You pay this higher premium for twice the number of years you delayed.
To learn how to avoid these extra charges, review Learn how to avoid financial penalties and How to Sign Up for Medicare Without Getting Penalized.
Navigating Coverage Start Dates and Gaps
Knowing when coverage starts after you enroll is just as important as knowing when you can enroll. A misunderstanding here can create a coverage gap.
Below is a simplified overview of when coverage typically begins for major enrollment periods:
| Enrollment Period | Dates | General Coverage Start Date |
|---|---|---|
| Initial Enrollment Period (IEP) | 7 months around your 65th birthday | Depends on when you enroll (see rules below). |
| Annual Enrollment Period (AEP) | October 15 – December 7 | January 1 of the following year. |
| Medicare Advantage OEP (MA OEP) | January 1 – March 31 | First day of the month after your new plan receives your enrollment request. |
| General Enrollment Period (GEP) | January 1 – March 31 | Generally the first day of the month after you enroll (rules can vary by year; check Medicare.gov). |
| Special Enrollment Periods (SEPs) | Varies by event | Generally the first day of the month after your enrollment request is received (event-specific rules may apply). |
IEP coverage timing basics:
- If you enroll in the three months before your birthday month, coverage usually starts the first day of your birthday month (or the month prior if your birthday is on the 1st)
- If you enroll during your birthday month, coverage starts the first day of the next month
- If you enroll in the three months after your birthday month, coverage is delayed, starting two or three months after you enroll
Understanding these timelines is crucial to avoid any gaps in your health coverage. For more details, see When does Medicare coverage start? and When Do You Need to Enroll in Medicare?.
Frequently Asked Questions about Medicare Enrollment Periods
We know Medicare can be confusing, and we often get asked similar questions. Let’s tackle some common concerns to make your enrollment journey smoother.
What happens if I’m happy with my current Medicare plan?
If you’re content with your current Medicare Advantage or Part D plan, you generally don’t need to do anything during the Annual Enrollment Period (AEP). Most plans will automatically renew for the following year.
However, it is critically important to review your Annual Notice of Change (ANOC) letter, which your plan sends out each fall. This document details any changes to your plan’s benefits, costs, or covered services for the upcoming year. For example, your prescription drug formulary might change, or your doctor might leave the network. Even if you love your plan now, these changes could make it less ideal for your needs next year. Reviewing your ANOC is a simple step that can save you a lot of headaches (and money!) later. Learn more about the Importance of Reviewing Your Annual Notice of Change Letters.
How do I enroll in Medicare?
Enrolling in Medicare Part A and Part B is primarily handled by the Social Security Administration (SSA). You have a few convenient ways to enroll:
- Online: The easiest way for many is to apply online at the Social Security website. You can Apply online at SocialSecurity.gov.
- By Phone: You can call the Social Security Administration directly at 1-800-772-1213 (TTY users can call 1-800-325-0778), Monday through Friday, 8:00 AM to 7:00 PM.
- In Person: You can visit your local Social Security office. We recommend calling ahead to make an appointment to avoid long wait times.
To enroll in a Medicare Advantage Plan (Part C) or a Medicare Part D Prescription Drug Plan, you’ll typically enroll directly through the private insurance company offering the plan. You can do this via their website, by phone, or with the help of a licensed insurance agent.
Can I change my mind after picking a plan?
Yes, you can often change your mind, but it depends on the type of plan you chose and which enrollment period you’re in.
- During the AEP (October 15 – December 7): You can make as many changes as you need during this period. The last valid election you make by December 7th will be the plan that takes effect on January 1st.
- During the MA OEP (January 1 – March 31): If you’re in a Medicare Advantage plan, you get one chance to switch to another Medicare Advantage plan or return to Original Medicare.
- Medigap Trial Right: If you enroll in a Medicare Advantage Plan when you first become eligible for Medicare and then decide to switch back to Original Medicare within the first 12 months, you have a special “trial right” to buy certain Medigap policies without medical underwriting. This is a crucial protection for those who try Medicare Advantage and decide it’s not for them.
- Special Enrollment Periods (SEPs): If you qualify for an SEP, you can make changes to your Medicare Advantage or Part D plan outside of these standard periods.
Always double-check the specific rules for disenrollment and new enrollment to ensure continuous coverage.
Get Help Navigating Your Medicare Options
Understanding all the nuances of Medicare enrollment periods explained can be challenging. Medicare is complex, and making the right choices for your health and financial future is important. You do not have to figure it out alone.
Free, Unbiased Medicare Enrollment Periods Explained
There are excellent resources available to help you make informed decisions, and many offer free, unbiased assistance:
- State Health Insurance Assistance Programs (SHIPs): These programs offer free, personalized counseling to Medicare beneficiaries. Counselors can help you understand your options, compare plans, and complete enrollment. Find your local SHIP at the SHIP website.
- Medicare.gov: The official Medicare website provides detailed information, plan comparison tools, and a live chat feature. Visit the Medicare.gov website to get started.
- We Can Help You, Inc.: As a non-profit dedicated to educating individuals on Medicare and Social Security for retirement, we provide free educational resources so you can confidently make decisions about your coverage. We also offer a free Medicare Planning Guide and a free Social Security maximization report to help you increase your retirement income.
If you’re in Arizona, California, Colorado, Connecticut, Florida, Georgia, Illinois, Indiana, Maine, Massachusetts, Michigan, Nebraska, Nevada, New Hampshire, New Jersey, New Mexico, New York, North Carolina, Ohio, Pennsylvania, Rhode Island, South Carolina, Tennessee, Texas, Vermont, or Virginia, we can connect you with local experts who understand the plans available in your area. For example, if you’re looking for assistance in Michigan, you can explore options like Find Medicare insurance agents near me in MI.
Making the right Medicare choices can impact your health and finances for years to come. Taking time to understand your Medicare enrollment periods now can help you get the coverage you need, when you need it, and avoid unnecessary penalties.



