Understanding Your Medicare Financial Responsibility
Medicare costs explained can feel overwhelming, but the basics are straightforward: you’ll pay four main types of expenses.
Quick Answer: The Four Types of Medicare Costs
- Premium – Monthly payment for your coverage
- Deductible – Amount you pay before Medicare starts paying
- Copayment – Fixed dollar amount per service (like $25 for a doctor visit)
- Coinsurance – Percentage of the cost you pay (like 20% of a medical bill)
Is Medicare free when you turn 65? No. Despite paying Medicare taxes throughout your working years, most people still pay premiums and cost-sharing when they use services. In fact, 29% of Medicare households in 2022 spent 20% or more of their total income on health-related costs, compared to just 7% of non-Medicare households.
Here’s what makes Medicare costs confusing: what you pay depends on which parts of Medicare you have, what services you need, and even how much income you earn. There’s also a critical detail many people miss – Original Medicare has no yearly limit on out-of-pocket costs unless you add supplemental coverage.
This guide breaks down exactly what you’ll pay for each part of Medicare, how your income affects your premiums, and how supplemental plans can protect you from unlimited expenses. You’ll get specific 2026 costs and learn where to find help making the right choices for your situation.
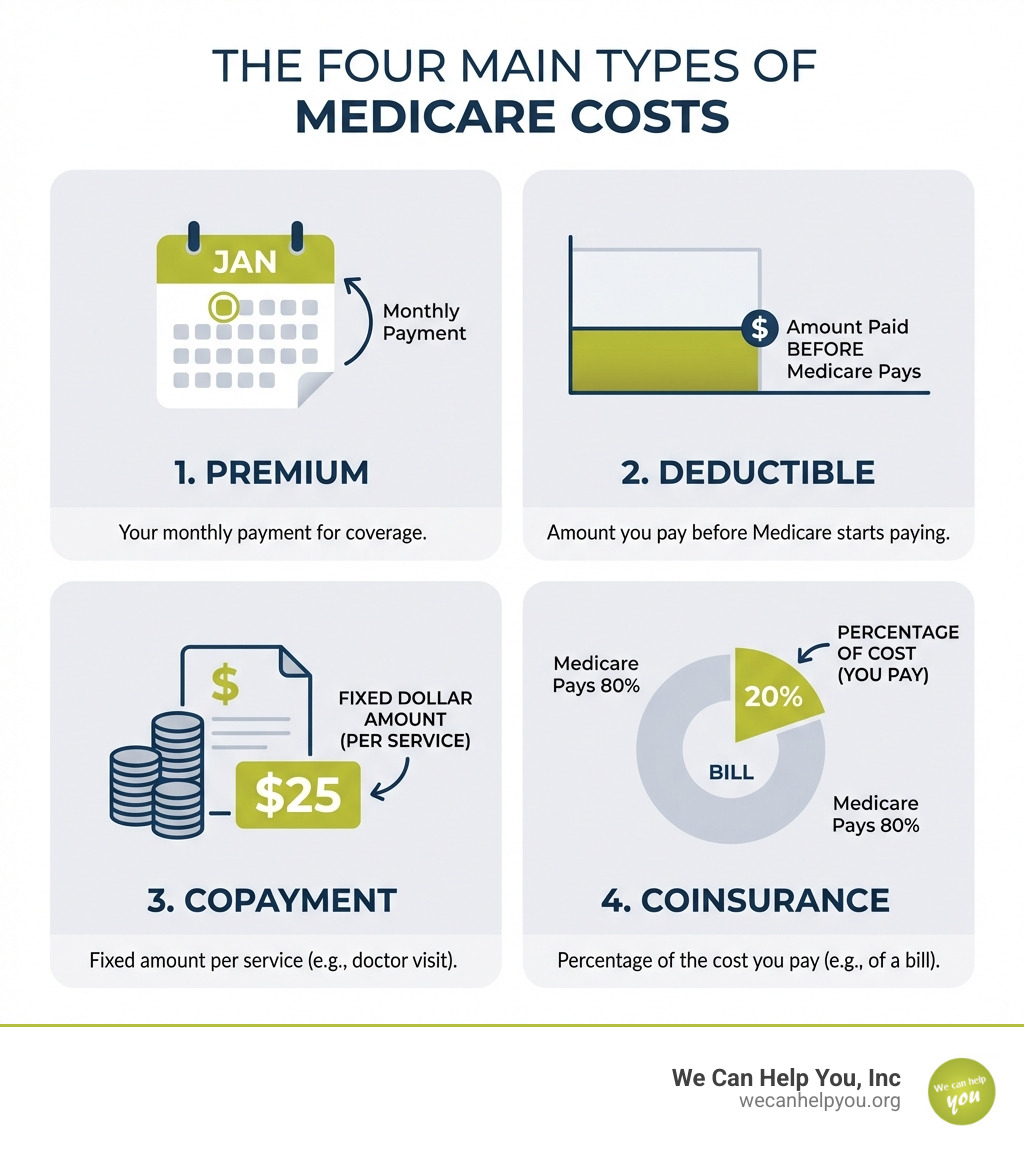
The Four Main Types of Medicare Costs
When we talk about Medicare costs explained, understand the basic financial terms involved. These are the building blocks of your healthcare expenses under Medicare, and knowing them empowers you to make informed decisions. What you pay for Medicare will vary based on what coverage and services you get, and what providers you visit. Let’s dig into the four main types of out-of-pocket costs you’ll encounter. You can learn more about these foundational costs at What does Medicare cost?.

What is a Premium?
Think of a premium as your monthly subscription fee for Medicare coverage. Just like you pay a monthly bill for your internet or streaming services, a premium is the amount you are required to pay each month to Medicare or your private insurer for your healthcare coverage.
- Part A Premium: While many people don’t pay a premium for Part A (more on this below), some individuals do. If you don’t qualify for premium-free Part A, you would pay a monthly premium.
- Part B Premium: Most people pay a standard monthly premium for Part B. This amount can change annually, and as we’ll discuss, it can be higher if you have a higher income.
- Part D Premium: If you enroll in a Medicare Prescription Drug Plan (Part D), you will pay a separate monthly premium to the private insurance company that offers the plan. The average estimated premium for Medicare Part D in 2025 is $46.50.
- Medicare Advantage Premium: Many Medicare Advantage (Part C) plans have a monthly premium in addition to your Part B premium. Some plans even offer a $0 premium, though you still pay your Part B premium.
Understanding how these premiums are structured is the first step in comprehending your overall Paying for Medicare Premiums.
What is a Deductible?
A deductible is the amount you pay for medical services or prescription drugs in a plan year before your plan begins to pay for benefits. It’s like the initial hurdle you clear before your insurance coverage fully kicks in.
- Part A Deductible: This applies per benefit period for hospital inpatient stays. For example, if you have a hospital stay covered under Part A in 2025, you will have to pay a deductible of $1,676 before your Medicare coverage kicks in. For 2026, this deductible is $1,736 per benefit period.
- Part B Deductible: This is an annual deductible. Once you meet it, Original Medicare generally pays 80% of the Medicare-approved amount for most doctor services and outpatient care. In 2026, the Part B deductible is $283.
- Part D Deductible: Most Part D plans have an annual deductible, though some plans may have a $0 deductible. You pay the full cost of your prescriptions until you meet this amount.
Deductibles are crucial because they represent a significant upfront cost you might incur before Medicare starts covering a larger portion of your medical bills.
What are Copayments and Coinsurance?
Copayments and coinsurance are both forms of cost-sharing, meaning you pay a portion of the cost for covered services after you’ve met your deductible. However, they differ in how that cost is calculated.
- Copayment (Copay): A copayment is a specific dollar amount you may be required to pay as your share of the cost for medical services or supplies. It’s a fixed amount. For example, you might have a $20 copay for a doctor’s office visit or a $10 copay for a prescription. An example from our research is paying $25 every time you see a specialist.
- Coinsurance: Coinsurance is a percentage of your medical and drug costs you may be required to pay as your share of costs for medical services or supplies. This means the amount you pay varies depending on the total cost of the service. For example, after meeting your Part B deductible, you typically pay 20% coinsurance for most doctor services and outpatient therapy. This means if a service costs $100, you pay $20, and Medicare pays $80.
The key difference: a copay is a fixed dollar amount, while coinsurance is a percentage. Both contribute to your out-of-pocket expenses for services.
Medicare Costs Explained by Part (A, B, C, and D)
Medicare is divided into different parts, each covering specific services and having its own cost structure. Understanding these parts is fundamental to grasping Medicare costs explained. Original Medicare includes Part A (Hospital Insurance) and Part B (Medical Insurance). Beyond that, you can choose to add Part D (Prescription Drug Coverage) or opt for a bundled plan like Medicare Advantage (Part C). To see a comprehensive overview of what Medicare covers, check out What does Medicare actually cover in 2025?.
Part A (Hospital Insurance) Costs Explained
Part A primarily covers inpatient hospital stays, skilled nursing facility care, hospice care, and some home health care.
- Premium-Free Part A: Good news for many! Most people don’t pay a monthly premium for Part A. You qualify for premium-free Part A if you or your spouse paid Medicare taxes through employment for at least 10 years (40 quarters). This is because your Medicare taxes essentially pre-paid your Part A premiums.
- Part A Premium Cost: If you don’t meet the 10-year work requirement, you might have to pay a monthly premium. For 2026, if you paid Medicare taxes for 30-39 quarters, your premium could be up to $278 per month. If you paid for fewer than 30 quarters, the premium could be as high as $565 per month.
- Hospital Inpatient Deductible: This is a significant cost. For a hospital inpatient stay, you pay a deductible per benefit period. A benefit period begins the day you’re admitted as an inpatient in a hospital or skilled nursing facility (SNF) and ends when you haven’t received inpatient hospital care or skilled care in an SNF for 60 days in a row. For 2026, this deductible is $1,736 per benefit period.
- Skilled Nursing Facility Costs: For skilled nursing facility stays, you pay $0 for the first 20 days of each benefit period in 2026. For days 21-100, you pay a daily coinsurance amount (for 2026, this is $217 per day). After day 100, you pay all costs.
These costs highlight that even with premium-free Part A, significant expenses can arise during hospitalizations or extended care. For more detailed information on these specific costs, you can visit Medicare Hospital Costs.
Part B (Medical Insurance) Costs Explained
Part B covers medically necessary services like doctor visits, outpatient care, preventive services, durable medical equipment, and some home health care.
- Standard Monthly Premium: For most beneficiaries, the government pays a substantial portion—about 75%—of the Part B premium, and the beneficiary pays the remaining 25%. The standard Part B monthly premium amount is $202.90 in 2026. This premium is typically deducted directly from your Social Security benefit.
- Part B Deductible: In 2026, the Part B deductible is $283 before Original Medicare starts to pay. You must pay this amount out of pocket each year before Medicare begins to cover your Part B services.
- 20% Coinsurance: After you meet your deductible, you generally pay 20% of the Medicare-approved amount for most doctor services (including most doctor services while you’re an inpatient in a hospital), outpatient therapy, and durable medical equipment. There’s no yearly limit on this 20% coinsurance under Original Medicare, which can lead to substantial costs for extensive medical care.
It’s important to be aware of these cost-sharing requirements, as they can add up, especially for ongoing treatments or frequent doctor visits. For more details on the 2026 premiums, check out 2026 Medicare Part B Premiums, and for outpatient costs, refer to Medicare Outpatient Costs.
Part D (Prescription Drug) Costs
Medicare Part D provides prescription drug coverage through private insurance companies approved by Medicare. Costs can vary significantly based on the plan you choose.
- Monthly Premium: You’ll pay a monthly premium directly to your Part D plan provider. This premium varies widely by plan and by location.
- Annual Deductible: Many Part D plans have an annual deductible, which you must pay before your plan starts to cover your prescription costs. This deductible can vary from plan to plan, up to a maximum set by Medicare.
- Copayments and Coinsurance: After meeting your deductible, you’ll pay copayments or coinsurance for your prescriptions. These costs typically depend on the drug’s tier (generic, preferred brand, non-preferred brand, specialty).
- National Base Premium: The Part D national base premium is an important figure, used in calculating late enrollment penalties and income-related monthly adjustment amounts (IRMAA). The 2026 Part D national base premium is $38.99.
It’s worth noting that the Inflation Reduction Act has brought significant changes to Part D costs, including capping insulin costs and eventually out-of-pocket spending for beneficiaries. You can find more information about these changes at Inflation Reduction Act Impact on Medicare Part D for 2025.
How Your Income Affects Your Premiums (IRMAA)
One of the most surprising aspects of Medicare costs explained for many beneficiaries is the Income-Related Monthly Adjustment Amount, or IRMAA. If your income is above certain thresholds, you’ll pay a higher premium for both Medicare Part B and Medicare Part D. This is a crucial detail for higher-income individuals to understand.
- What is IRMAA? IRMAA is an additional premium amount that individuals with higher incomes pay for their Medicare Part B and Medicare prescription drug coverage. The law requires an adjustment to these monthly premiums based on your Modified Adjusted Gross Income (MAGI).
- How it’s Determined: Social Security uses the most recent federal tax return information provided by the IRS, specifically your MAGI, to determine if you are a higher-income beneficiary. Your MAGI includes your adjusted gross income plus tax-exempt interest income.
- Part B IRMAA: For most beneficiaries, the government covers about 75% of the Part B premium, and you pay the remaining 25%. However, if your income is above the specified thresholds, you could pay 35%, 50%, 65%, 80%, or even 85% of the total Part B cost, depending on your income bracket.
- Part D IRMAA: Similarly, if your income is above the thresholds, you will pay an additional amount for your Part D prescription drug coverage premium. This is added to your plan’s premium.
Income Thresholds (for 2026, based on 2024 tax returns):
| Filing Status | MAGI (Individual) | MAGI (Married Filing Jointly) | Part B Premium Increase (2026) | Part D Premium Increase (2026) |
|---|---|---|---|---|
| Individual/Married Filing Separately | > $109,000 | N/A | $81.20 – $487.90 | $14.50 – $91.00 |
| Married Filing Jointly | N/A | > $218,000 | $81.20 – $487.90 | $14.50 – $91.00 |
Note: The exact premium increase depends on specific income brackets within these ranges.
- Life-Changing Events: What if your income has gone down due to a major life-changing event? Social Security understands that circumstances change. If your income has decreased due to events like marriage, divorce, death of a spouse, work stoppage, work reduction, loss of income-producing property, or loss of a pension, you can contact Social Security to report the new information. You may need to use Form SSA-44 to request a new decision on your IRMAA.
- Appealing a Decision: If you disagree with Social Security’s IRMAA decision, you have the right to appeal. You can file an appeal online, in writing, or by contacting your local Social Security office.
Understanding IRMAA is vital for financial planning, as it can significantly impact your monthly Medicare expenses. For a deeper dive, read our guide on Understanding Medicare IRMAA Charges.
Managing Your Out-of-Pocket Expenses
One of the most critical insights when discussing Medicare costs explained is a stark reality: Original Medicare (Parts A and B) does not have a yearly limit on your out-of-pocket expenses. This means that if you have extensive medical needs, your costs could theoretically be unlimited. This is where supplemental coverage becomes invaluable.
The Risk of No Yearly Limit with Original Medicare
Imagine facing a serious illness or a prolonged hospital stay. Under Original Medicare, after you meet your deductibles, you’re generally responsible for 20% coinsurance for most Part B services and significant daily coinsurance amounts for extended Part A hospital or skilled nursing facility stays. Without a yearly cap, these costs can quickly accumulate, potentially leading to unlimited financial exposure. For individuals with chronic conditions or those who experience unexpected illnesses, this can result in incredibly high medical bills that could jeopardize their financial security. This is why it’s so important to consider how to protect yourself from these potentially uncapped costs.
How Supplemental Plans Limit Your Costs
Fortunately, you have options to cap your out-of-pocket expenses: Medigap policies and Medicare Advantage Plans. Understanding the differences between these can help you manage your financial risk. You can explore the distinctions further at Medicare Advantage vs Medigap.
- Medigap Policies (Medicare Supplement Insurance): These are private insurance policies that help pay for some of the costs that Original Medicare doesn’t cover, such as copayments, coinsurance, and deductibles. They are “standardized,” meaning plans of the same letter (e.g., Plan G) offer the same basic benefits, regardless of the insurance company. Medigap policies significantly reduce your out-of-pocket costs, but they do not typically have an annual out-of-pocket maximum themselves; rather, they fill in the gaps so you pay less or nothing for covered services.
- Medicare Advantage (Part C) Plans: These plans are offered by private insurance companies approved by Medicare. They provide all your Part A and Part B benefits, and often include Part D prescription drug coverage and additional benefits like dental, vision, and hearing. A key feature of all Medicare Advantage plans is an annual out-of-pocket maximum. Once you reach this limit, the plan pays 100% of your covered medical costs for the rest of the year. This provides a crucial financial safety net. Some Medicare Advantage plans even offer $0 Premium Plans, though you still pay your Part B premium. For a deeper dive into these options, read our guide on Understanding the differences between Medigap and Medicare Advantage.
Choosing a supplemental plan can provide peace of mind by limiting your financial exposure and making your healthcare costs more predictable.
A Look Ahead: Key Medicare Costs in 2026
To give you a clearer picture of your potential expenses, let’s look at some of the key Medicare costs explained for the upcoming year, 2026. That these figures can be adjusted annually, but they provide a solid estimate for planning purposes. For the most up-to-date information, always refer to official Medicare resources. You can also explore our own insights on 2026 Medicare Costs and find out Will my Medicare premiums rise in 2026?.
Medicare Part A (Hospital Insurance) Costs for 2026:
- Part A Premium (if not premium-free): Up to $565 per month (if you paid Medicare taxes for fewer than 30 quarters).
- Part A Deductible: $1,736 per benefit period for hospital inpatient stays.
- Part A Coinsurance for Hospital Stays:
- Days 1-60: $0
- Days 61-90: $434 per day
- Days 91 and beyond (lifetime reserve days): $868 per day (up to 60 lifetime reserve days)
- Part A Coinsurance for Skilled Nursing Facility Stays:
- Days 1-20: $0
- Days 21-100: $217 per day
- Days 101 and beyond: All costs
Medicare Part B (Medical Insurance) Costs for 2026:
- Standard Part B Premium: $202.90 per month. This amount can be higher if you are subject to IRMAA due to higher income.
- Part B Deductible: $283 per year.
- Part B Coinsurance: Generally 20% of the Medicare-approved amount for most doctor services and outpatient care after your deductible is met.
Medicare Part D (Prescription Drug) Costs for 2026:
- Part D National Base Premium: $38.99 per month. This figure is used for calculating IRMAA and late enrollment penalties, not necessarily your plan’s actual premium. Your individual plan premium will vary.
- Part D Deductible, Copayments, and Coinsurance: These costs will vary significantly by the specific plan you choose.
These projected costs for 2026 underscore the importance of ongoing financial planning and understanding your coverage choices.
Where to Get Help with Your Medicare Costs
Navigating the complexities of Medicare costs explained can be challenging, but you don’t have to do it alone. There are numerous resources available to help you understand your options, manage your expenses, and even find programs to assist with costs.
- Official Medicare Resources: The official Medicare website, Medicare.gov, is an excellent starting point. It offers comprehensive information on all aspects of Medicare, including detailed cost breakdowns for different services. You can also call 1-800-MEDICARE (1-800-633-4227; TTY 1-877-486-2048) for direct assistance.
- The Medicare & You Handbook: This annual publication is your official guide to Medicare. It provides detailed information on what Medicare covers, your costs, and your rights. You can easily access and read the Medicare & You Handbook online.
- State Health Insurance Assistance Programs (SHIP): SHIPs offer free, impartial, and personalized counseling to Medicare-eligible older adults, their families, and caregivers. These programs are invaluable for helping you sort through your Medicare options and understand your costs. Our research shows that contacting a SHIP office is a highly recommended actionable step for beneficiaries. To find your local SHIP office, you can call 1-877-839-2675 or use the online SHIP locator.
- Social Security Administration (SSA): For questions related to Medicare Part B premiums, IRMAA, or if you need to report a life-changing event affecting your income, the Social Security Administration is your go-to resource. You can call them at 1-800-772-1213.
- Programs to Help with Costs: There are federal and state programs designed to help individuals with limited income and resources pay for Medicare premiums and other costs. These include Medicaid, Medicare Savings Programs (MSPs), and Extra Help for prescription drug costs. In many of the states where we operate, such as Arizona, California, Florida, Illinois, New York, and Texas, these programs can provide significant financial relief. Your local SHIP counselor can help you determine if you qualify for any of these programs.
We understand that navigating Medicare can be complex, and finding the right information can sometimes feel like a treasure hunt. These resources are designed to simplify that process and ensure you get the support you need.
Conclusion
Understanding Medicare costs explained is more than just knowing numbers; it’s about gaining peace of mind and making informed decisions about your healthcare and financial future. We’ve explored the four main types of costs—premiums, deductibles, copayments, and coinsurance—and digd into how these apply across Medicare Parts A, B, and D. We’ve also highlighted the critical impact of income-related adjustments (IRMAA) and the vital role supplemental plans play in protecting you from unlimited out-of-pocket expenses.
Medicare is not free, and your specific costs will depend on your chosen coverage, your healthcare needs, and your income. While the system can seem intricate, resources like the Medicare website, the Medicare & You Handbook, and especially State Health Insurance Assistance Programs (SHIPs) are there to guide you.
At We Can Help You, Inc., we are dedicated to educating individuals on Medicare and Social Security for retirement. We believe that understanding these complex systems shouldn’t be a burden. That’s why we offer resources to help you confidently manage your retirement healthcare and income.
Don’t leave your Medicare costs to chance. Take the next step towards a secure retirement.