Is Medicare Advantage Right for You? Here’s What You Need to Know
Medicare Advantage explained simply: it’s an alternative way to get your Medicare coverage through a private insurance company instead of directly through the federal government.
Here’s a quick summary of the key facts:
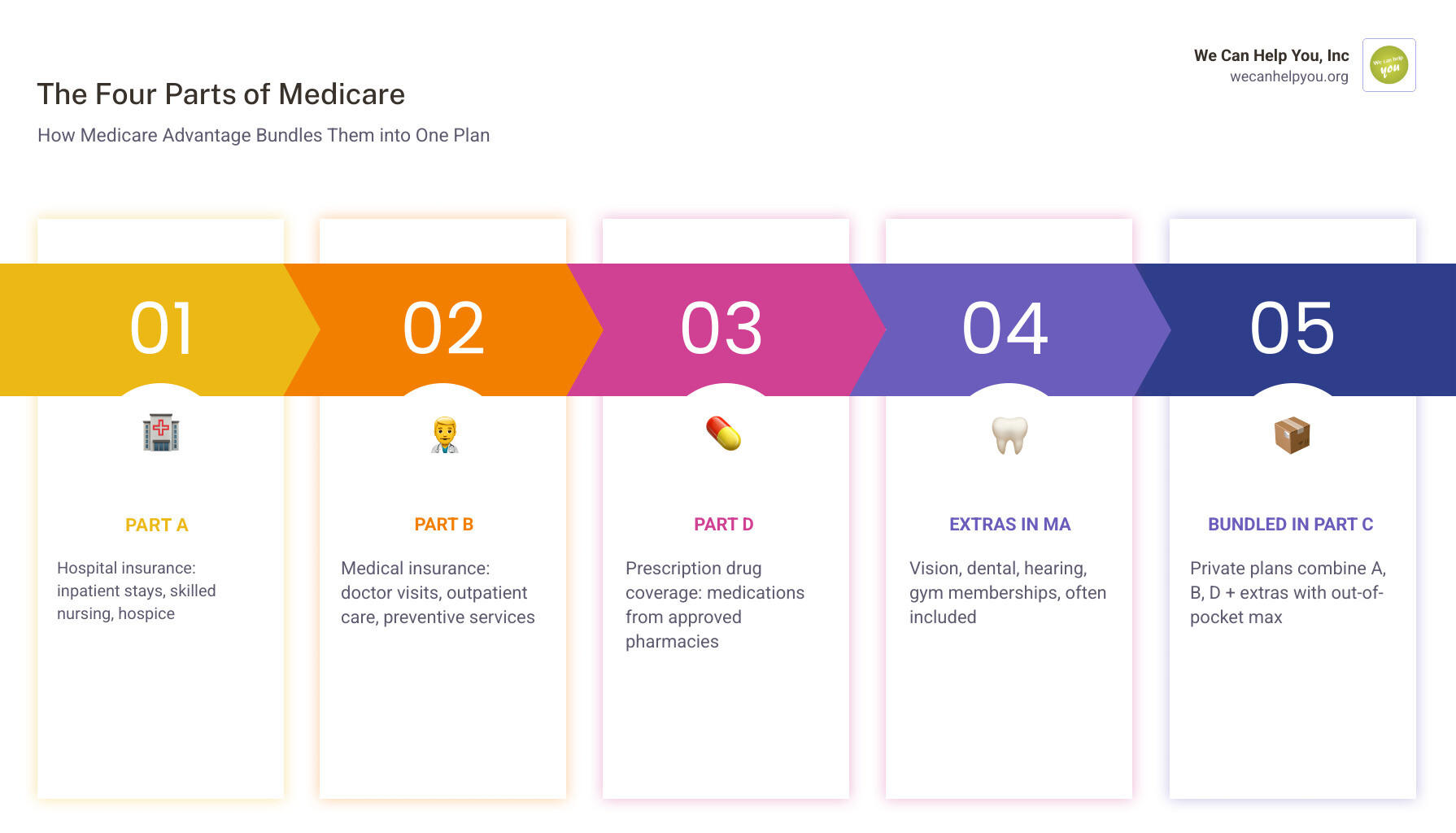
- What it is: Medicare Advantage (also called Part C) bundles your hospital coverage (Part A), medical coverage (Part B), and usually prescription drug coverage (Part D) into one private health plan
- Who runs it: Medicare-approved private insurance companies — not the government directly
- Extra perks: Many plans include vision, dental, hearing, and even non-medical benefits like gym memberships
- The tradeoff: You typically must use the plan’s network of doctors and may need prior authorization for some services
- The cost: Most people pay the standard Part B premium ($202.90/month in 2026), plus a plan premium that averages just $14/month — and many plans charge $0 in additional premium
- Out-of-pocket protection: Unlike Original Medicare, every Medicare Advantage plan has a yearly spending cap
Medicare is already complicated. Add Social Security timing, retirement income planning, and dozens of plan choices — and it’s easy to feel stuck.
You’re not alone. In 2023, nearly half of all Medicare beneficiaries (49%) were enrolled in Medicare Advantage plans, and that number keeps climbing. Clearly, it’s worth understanding before you decide.
This guide breaks everything down in plain language so you can make a confident, informed choice.
What is Medicare Advantage? (Medicare Advantage Explained)
When we talk about medicare advantage explained, the first thing to understand is that it is not a “supplement” to your government insurance. Instead, it is a replacement for how you receive your benefits. While Original Medicare is managed by the federal government, Medicare Advantage (Part C) is a way for you to receive those same benefits through a private insurance company.
Think of it like choosing between a public utility and a private service provider. Both provide the electricity (your healthcare), but the private provider might offer different “packages” or “bundles.” According to the Official Medicare Advantage definition, these plans must cover everything that Original Medicare covers, but they do so under a single umbrella.
By law, these plans are strictly regulated by the Centers for Medicare & Medicaid Services (CMS). Even though a private company like UnitedHealthcare or Aetna might be the name on your card, the government still sets the rules. This ensures you have Medicare Advantage basics covered, such as emergency care and medically necessary hospital stays.
How Medicare Advantage Works
Medicare Advantage plans operate on a “capitation” model. This is a fancy way of saying that the government pays the private insurance company a fixed monthly amount to take care of you. In exchange, the insurance company assumes the financial risk for your health.
Because the insurance company is managing your care, they use Medicare Part C rules to stay profitable while keeping you healthy. This usually involves:
- Using a specific network of doctors and hospitals.
- Requiring referrals for specialists.
- Using “managed care” techniques to ensure treatments are medically necessary.
Eligibility for Medicare Advantage Explained
To join a Medicare Advantage plan, you generally need to meet three simple criteria:
- You must be enrolled in both Medicare Part A (Hospital) and Part B (Medical).
- You must live in the plan’s service area (usually your county).
- You must be a U.S. citizen or be lawfully present in the country.
The popularity of these plans is skyrocketing. In 2023, 49 percent of Medicare beneficiaries chose Medicare Advantage, and experts project that by 2025, more than half of all people on Medicare will be in a Part C plan. This trend is driven by the desire for “all-in-one” coverage and the predictable costs that these plans offer.
Comparing Medicare Advantage vs. Original Medicare
Deciding between these two paths is the most important choice you’ll make in your Medicare journey. Original Medicare offers ultimate freedom—you can see any doctor in the U.S. that accepts Medicare. Medicare Advantage offers “coordinated care”—you stay within a network but often get more benefits for a lower monthly cost.
| Feature | Original Medicare | Medicare Advantage |
|---|---|---|
| Provider Choice | Any doctor in the U.S. accepting Medicare | Usually limited to plan network |
| Drug Coverage | Must buy a separate Part D plan | Usually included in the bundle |
| Out-of-Pocket Limit | None (No cap on spending) | Yes (Annual cap on spending) |
| Extra Benefits | Generally none (No dental/vision) | Vision, Dental, Hearing, Fitness |
| Referrals | Usually not required | Often required for specialists |
One of the biggest differences involves supplemental insurance. When you have Original Medicare, you can buy a Medigap policy to help pay for the 20% coinsurance that Medicare doesn’t cover. However, when looking at Medicare Advantage vs Medigap, you cannot have both. If you choose Medicare Advantage, you are choosing to forgo Medigap. Understanding the Differences Between Medigap and Medicare Advantage is key to avoiding expensive mistakes during enrollment.
Provider Networks and Prior Authorization
The “trade-off” for the extra benefits in Medicare Advantage is the Provider Network. Unlike Original Medicare, where you have a “nationwide” network, a 2017 analysis found that Medicare Advantage networks included fewer than half (46%) of all Medicare physicians in a given county, on average.
Furthermore, you will often encounter Prior Authorization. This means your doctor must get approval from the insurance company before performing certain procedures or prescribing expensive drugs. While this helps control costs, a recent government report found that about 13% of prior authorization denials were for care that actually met Medicare coverage rules. This is why we always recommend checking if your favorite doctors are “in-network” before you sign up.
Extra Benefits Beyond Original Medicare
Why do so many people switch? It’s the “extras.” Original Medicare famously does not cover routine dental, vision, or hearing care. Medicare Advantage plans fill these gaps. In our Medicare Advantage: Your Guide to Benefits and Drawbacks, we highlight that these perks can save you thousands of dollars a year.
Common extra benefits include:
- Vision: Exams, frames, and contact lenses.
- Dental: Cleanings, X-rays, and sometimes even dentures or crowns.
- Hearing: Exams and subsidized hearing aids.
- Wellness: Free gym memberships (like SilverSneakers).
- Non-Medical Perks: Some plans now offer grocery allowances, utility bill assistance, or transportation to doctor appointments for those who qualify.
Types of Medicare Advantage Plans Available
Not all Part C plans are the same. Depending on where you live—whether it’s Florida, Texas, or New York—you will likely see several different “flavors” of plans.

- Health Maintenance Organization (HMO): These are usually the most affordable but the most restrictive. You must stay in the network and you usually need a referral from a primary care doctor to see a specialist.
- PPO (Preferred Provider Organization): These offer more flexibility. You can see out-of-network doctors, but you’ll pay a higher copay or coinsurance for doing so.
- Private Fee-for-Service (PFFS): These plans determine how much they will pay providers and how much you must pay. You can see any provider who agrees to the plan’s terms.
- Medical Savings Accounts (MSA): These combine a high-deductible health plan with a bank account. Medicare deposits money into the account to help you pay for healthcare.
Special Needs Plans (SNPs) for High-Need Beneficiaries
There is a special category of Medicare Advantage for those who need extra help. More than 6 million beneficiaries in SNPs receive care tailored to their specific situation.
- C-SNPs: For people with chronic conditions like diabetes or heart failure.
- D-SNPs: For “dual-eligible” individuals who have both Medicare and Medicaid.
- I-SNPs: For people living in an institution (like a nursing home).
Understanding the Costs of Medicare Advantage
When people ask for medicare advantage explained, they usually want to know about the “catch” with the price. You might see advertisements for “$0 premium” plans and wonder: How Can Medicare Advantage Part C Plans Be 0 Premium?
The reality is that while the plan premium might be $0, you still have to pay your monthly Medicare Part B premium ($202.90 in 2026). The insurance company can offer a $0 premium because they are being paid by the government to manage your care.
Other costs to watch for:
- Deductibles: The amount you pay before the plan starts to kick in.
- Copayments: A flat fee (e.g., $20) for a doctor visit.
- Coinsurance: A percentage (e.g., 20%) of the cost for a service.
Out-of-Pocket Maximums and Financial Protection
The single biggest financial “pro” of Medicare Advantage is the out-of-pocket maximum. In Original Medicare, if you have a catastrophic illness, you could theoretically owe hundreds of thousands of dollars because there is no cap on that 20% coinsurance.
In 2024, the government set the maximum out-of-pocket limit at $8,850 in-network limit. Once you hit that number, the plan pays 100% of your covered medical costs for the rest of the year. This provides a level of financial predictability that Original Medicare simply doesn’t offer without an expensive Medigap policy.
Medicare Star Ratings and Plan Quality
How do you know if a plan is actually good? The government uses Medicare Star Ratings to grade plans on a scale of 1 to 5 stars. These ratings are based on customer service, how well the plan manages chronic conditions, and member satisfaction.
Understanding How CMS Determines Star Ratings for Medicare Part C and Part D Plans can help you filter out the low-performing plans. In 2023, about 71% of enrollees were in plans with 4 or more stars. We always recommend looking for a 4-star plan or higher to ensure you’re getting quality care.
When to Enroll: Medicare Advantage Enrollment Periods Explained
You can’t just join a plan whenever you feel like it. You have to wait for specific windows of time.
- Initial Enrollment Period (IEP): The 7-month window when you first become eligible for Medicare (usually around your 65th birthday).
- Annual Enrollment Period (AEP): Every year from October 15 to December 7. This is when you can join, switch, or drop a plan.
- Medicare Advantage Open Enrollment Period (MA OEP): From January 1 to March 31. If you are already in a Medicare Advantage plan, you can switch to a different one or go back to Original Medicare. Knowing What to Do During the Medicare Advantage Open Enrollment Period is vital if you realize in January that your current plan doesn’t cover your new prescription.
- Special Enrollment Periods (SEP): These are triggered by life events, like moving to a new state (e.g., moving from New Jersey to North Carolina) or losing employer coverage.
Frequently Asked Questions about Medicare Advantage
Can I have Medigap and Medicare Advantage at the same time?
No. It is actually illegal for an insurance agent to sell you a Medigap policy if they know you are enrolled in a Medicare Advantage plan. They serve two different purposes. Medigap “wraps around” Original Medicare, while Medicare Advantage replaces it. If you try to use both, one will likely deny your claims.
Does Medicare Advantage cover prescription drugs?
Most do. These are often called MAPD plans (Medicare Advantage Prescription Drug plans). They bundle Part D coverage directly into the plan. You’ll want to check the plan’s “formulary” (drug list) to make sure your specific medications are covered and to see which pharmacy network you need to use.
What happens if I travel outside the United States?
Original Medicare generally does not cover you outside the 50 states. Some Medicare Advantage plans offer emergency and urgent care coverage worldwide as an extra benefit. However, if you travel frequently, you should look closely at the plan’s summary of benefits. For unbiased help, you can always contact the State Health Insurance Assistance Program (SHIP) help for free counseling on travel-friendly options.
Conclusion
We hope this has helped get medicare advantage explained in a way that makes sense for your future. Whether you prioritize the freedom of Original Medicare or the bundled perks and cost-caps of Medicare Advantage, the choice is ultimately about what makes you feel most secure in retirement.
At We Can Help You, Inc., we are a non-profit dedicated to making sure you don’t leave money on the table. Choosing the right health plan is just one piece of the puzzle. To truly maximize your retirement, you need to look at the big picture.
We invite you to take advantage of our free resources:
- Free Medicare Planning Guide: A step-by-step roadmap to navigate these choices.
- Free Social Security Maximization Report: Learn how to time your benefits to increase your lifetime retirement income.
Don’t guess when it comes to your health and your wealth. Whether you want to Compare Medicare Advantage vs Medigap or figure out your enrollment window, we are here to help. Contact us today to secure your retirement peace of mind.



