Understanding Medicare’s Daily Hospice Payments
How much does Medicare pay hospice per day? Medicare pays hospice providers daily rates that vary by level of care. These rates are updated annually. For example, recent rates for routine home care were $225 per day for the first 60 days and $177 per day thereafter. During crisis periods, continuous home care paid up to $1,619 per day, general inpatient care paid $1,170 per day, and respite care paid $519 per day.
Quick Reference: Example Medicare Hospice Daily Rates
(Note: Rates are updated annually by Medicare and may vary. The figures below are for illustrative purposes.)
| Level of Care | Example Daily Rate | When It’s Used |
|---|---|---|
| Routine Home Care (Days 1-60) | $225 | Standard home-based hospice care |
| Routine Home Care (Days 61+) | $177 | Ongoing home-based hospice care |
| Continuous Home Care | Up to $1,619 | Crisis periods requiring 8+ hours of care |
| General Inpatient Care | $1,170 | Short-term facility care for symptom management |
| Inpatient Respite Care | $519 | Temporary facility care to give caregivers a break |
When you or a loved one faces a terminal illness, understanding how Medicare covers hospice care becomes essential. The Medicare hospice benefit operates on a per-diem payment system, meaning providers receive a flat daily rate regardless of how many services they deliver on any given day.
This isn’t the traditional fee-for-service model you might be familiar with. Instead, Medicare pays hospice agencies one set amount each day to cover all care related to your terminal illness—from nursing visits and pain medications to counseling and medical equipment.
The payment amount depends on which of four levels of care you need. Most people receive routine home care about 98% of the time, but Medicare also covers more intensive care during crisis periods or when caregivers need temporary relief.
These daily rates are designed to support palliative care—comfort and symptom management—rather than treatments aimed at curing your illness. Once you elect the hospice benefit, you agree to focus on quality of life instead of curative treatments, though Medicare continues covering care for conditions unrelated to your terminal diagnosis.
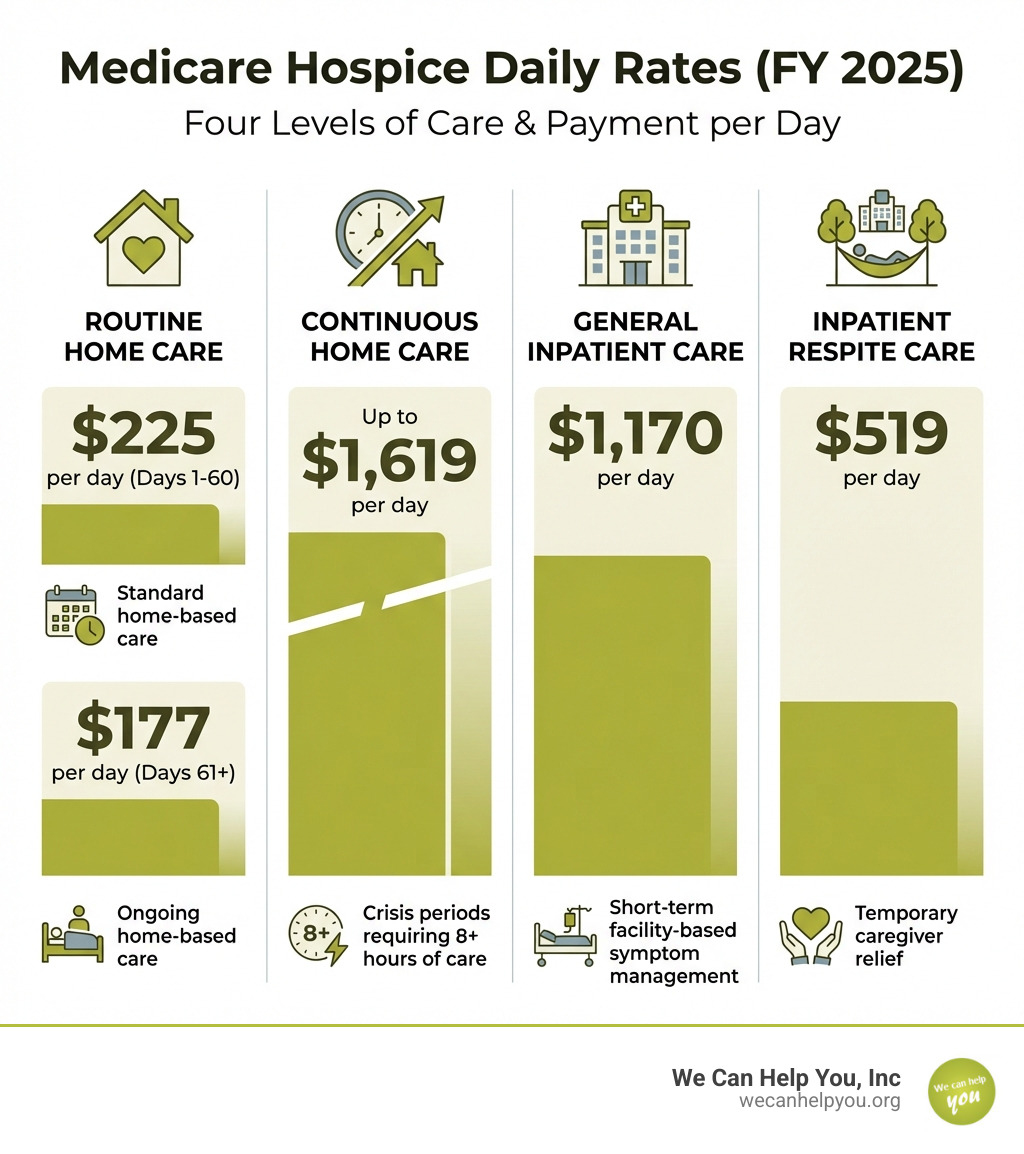
The Four Levels of Medicare Hospice Care and Their Daily Rates
Medicare Part A, often called Hospital Insurance, is the part of Medicare that covers hospice care. When a beneficiary chooses hospice, Medicare pays the hospice provider a daily rate to cover all services outlined in the patient’s personalized hospice plan of care. This means that for each day you are enrolled in hospice, the hospice agency receives a set amount, regardless of the number of services provided on that specific day—even on days when no direct services are provided.
These daily rates are set by Medicare each fiscal year and vary significantly based on the level of care needed. Understanding these levels is key to grasping how much Medicare pays hospice per day. Let’s explore the four distinct levels of care and their corresponding rates. For a deeper dive into what hospice care entails, visit our resources on Hospice Care.
Here’s a breakdown of example base payment rates for each level of care:
(Note: These rates are for a recent fiscal year and are updated annually.)
| Level of Care | Example Base Payment Rate (Daily) |
|---|---|
| Routine Home Care (Days 1-60) | $225 |
| Routine Home Care (Days 61+) | $177 |
| Continuous Home Care (CHC) | $1,619 |
| General Inpatient Care (GIC) | $1,170 |
| Inpatient Respite Care (IRC) | $519 |
What is Routine Home Care (RHC)?
Routine Home Care (RHC) is by far the most common level of hospice care, accounting for about 98 percent of all hospice days. This is the standard level of care provided to beneficiaries in their own residence, whether that’s a private home, an assisted living facility, or a nursing home.
Under RHC, the hospice agency provides all necessary services for the terminal illness and related conditions. This typically includes nursing services, hospice aide visits for personal care, medical supplies, equipment, and medications for symptom management and pain relief. Essentially, it covers everything needed to manage symptoms and provide comfort in the familiar surroundings of home.

What is Continuous Home Care (CHC)?
Continuous Home Care (CHC) is a more intensive level of support provided during periods of crisis. Imagine a situation where a patient experiences uncontrolled pain or severe symptoms that require continuous observation and care to avoid hospitalization. That’s when CHC steps in.
To qualify for CHC, a patient must receive a minimum of 8 hours of skilled care within a 24-hour period, with nursing care typically making up the majority of these hours. The goal is to manage acute symptoms at home and provide continuous support until the crisis subsides. While it’s paid as a daily rate, it’s calculated based on an hourly rate for the skilled services provided.
What is General Inpatient Care (GIC)?
General Inpatient Care (GIC) is for short-term stays in an inpatient facility, such as a hospice inpatient unit, hospital, or skilled nursing facility. This level of care is necessary when a patient’s symptoms (like severe pain, unmanaged nausea, or respiratory distress) cannot be managed effectively at home.
GIC focuses on intensive pain control and symptom management that requires the expertise of an inpatient setting until the symptoms are stabilized. Once symptoms are under control, the patient typically returns home for RHC.
What is Inpatient Respite Care (IRC)?
Inpatient Respite Care (IRC) is a real lifesaver for family caregivers. Providing continuous care for a loved one with a terminal illness can be emotionally and physically exhausting. IRC allows the primary caregiver to take a much-needed break.
During IRC, the beneficiary receives care in a Medicare-approved inpatient facility (like a hospice inpatient unit, hospital, or skilled nursing facility) for a short period, typically up to 5 consecutive days. This temporary stay provides relief for the caregiver while ensuring the patient continues to receive high-quality hospice care. While Medicare covers the bulk of the cost, beneficiaries may have a small coinsurance for IRC, which we’ll discuss later. For more details on the scope of hospice services, you can refer to More on hospice services.
How Much Does Medicare Pay Hospice Per Day? A Detailed Breakdown
Medicare’s hospice payment system is designed to incentivize quality care while managing costs. It employs a two-tiered payment system for routine home care and includes special adjustments for intense care needs at the very end of life. This structure helps ensure that hospice providers can deliver comprehensive support when it’s most needed.
Beyond the base daily rates, Medicare also offers additional payments, like the Service Intensity Add-on (SIA), to encourage timely and frequent visits by registered nurses and social workers during a patient’s final days. This recognition of the heightened needs during the last week of life reflects Medicare’s commitment to supporting both the patient and their family.
How much does Medicare pay hospice per day for routine care?
For Routine Home Care (RHC), Medicare uses a tiered system that adjusts the payment based on the length of time a patient has been receiving hospice services. The idea is that patients often have higher care needs at the beginning of their hospice journey, which may then stabilize.
- Days 1-60: For the first 60 days of hospice care, Medicare pays a higher daily rate. As an example, a recent base rate was approximately $225 per day.
- Days 61+: After the initial 60 days, the daily payment rate for RHC decreases. A recent base rate for this period was approximately $177 per day.
This tiered system acknowledges that the intensity of services may be greater during the initial phase of hospice enrollment as the care team establishes the plan of care, manages initial symptoms, and helps the family adjust. It’s a pragmatic approach to align payments with typical care patterns.
What is the Service Intensity Add-On (SIA)?
The Service Intensity Add-on (SIA) is an additional payment designed to support and encourage more frequent nursing and social work visits during a particularly critical time: the last seven days of a patient’s life. This add-on payment is provided in addition to the RHC daily rate.
- Eligibility: The SIA applies only to RHC days during the last seven days of life.
- Services Covered: It specifically covers direct patient care provided by a Registered Nurse (RN) or Social Worker (SW).
- Payment Structure: The SIA payment is an hourly rate that is updated annually. For example, a recent SIA rate was approximately $67 per hour for these visits, up to a maximum of four hours per day.
This means that if a patient receives RHC and has RN or SW visits in their final week, the hospice provider receives the standard RHC daily rate plus an hourly payment for those specific visits. It’s Medicare’s way of recognizing the crucial role these professionals play in providing comfort and support during a patient’s most vulnerable time.
Higher-Level Care and Payment Adjustments
Sometimes, the journey through a terminal illness involves periods of intense need that go beyond routine home care. Medicare’s payment system is designed to accommodate these situations, offering higher daily rates for crisis management and inpatient care. These rates are also subject to adjustments based on location and provider compliance.

How much does Medicare pay hospice per day for inpatient care?
When symptoms become too severe to manage at home, or when caregivers need a critical break, Medicare provides for inpatient hospice care.
- General Inpatient Care (GIC): Medicare pays a high daily rate for GIC, which is updated annually. A recent rate was approximately $1,170 per day. This rate covers the intensive, short-term care provided in a facility to bring acute symptoms under control. It’s a significant jump from routine home care, reflecting the higher resources required to manage a medical crisis effectively.
- Inpatient Respite Care (IRC): For IRC, Medicare also sets an annual rate. A recent rate was approximately $519 per day. This rate helps cover the cost of a patient’s temporary stay in a facility, offering respite to their primary caregiver. While Medicare covers most of this, beneficiaries may pay a 5% coinsurance for respite care, which can vary but is capped at the annual Part A inpatient hospital deductible.
When is Continuous Home Care (CHC) provided?
Continuous Home Care (CHC) is specifically reserved for acute symptom management at home, aiming to prevent unnecessary hospitalizations. It’s deployed during a patient crisis when intense, continuous care is required for 8 or more hours within a 24-hour period.
- Purpose: CHC is used when a patient experiences uncontrolled pain, severe nausea, or other acute symptoms that require constant skilled observation and care.
- Payment Structure: While the daily maximum payment is updated annually, a recent maximum was approximately $1,619. This is calculated based on an hourly rate (for example, about $67 per hour) for the skilled services provided. A significant portion of these hours must be nursing care.
This level of care allows patients to remain in their familiar home environment even during a crisis, with the assurance that skilled professionals are there around the clock to manage their symptoms.
Are daily payment rates ever reduced?
Yes, there are circumstances under which Medicare’s daily payment rates to hospice providers can be reduced. These reductions are primarily tied to provider compliance and geographic factors.
- Quality Reporting Compliance: To encourage high standards of care, Medicare requires hospice providers to submit specific quality data. Hospices that fail to comply with these quality data submission requirements face a penalty. For example, a recent penalty resulted in a 4% reduction to their annual payment update. This means their daily rates would be lower than those of compliant providers.
- Geographic Wage Index: Medicare adjusts the labor portion of its daily payments to account for differences in local wage rates across the country. This is done using a “hospice wage index.” For example, a hospice in a high-wage area like New York City might receive a higher payment for the labor component of care than a hospice in a lower-wage rural area. The wage index is applied to the labor share of the base payment amount for each level of care. This ensures that payments reflect the actual cost of employing staff in different regions. You can find detailed information on these requirements at Official Medicare coverage rules.
Understanding the Bigger Picture: Caps, Costs, and Coverage Rules
Beyond the daily rates, it’s important to understand the broader financial landscape of Medicare hospice benefits. This includes annual payment limits for providers, potential out-of-pocket costs for beneficiaries, and how hospice care interacts with different Medicare plans.
What is the annual hospice aggregate cap?
Medicare places an annual limit on the total amount of money a hospice provider can receive for services furnished to its beneficiaries. This is known as the annual hospice aggregate cap. It’s designed to prevent excessively long hospice stays that might not truly align with the terminal illness prognosis.
- How it works: The cap is calculated by multiplying a specific cap amount, which Medicare updates each year, by the number of Medicare beneficiaries served by that hospice in a given cap year.
- Example Cap Amount: As an example, a recent aggregate cap amount was approximately $34,465 per patient.
- Impact: If a hospice’s total payments from Medicare for the year exceed this aggregate cap, the hospice must repay the overage to Medicare. This mechanism encourages hospices to manage care efficiently and ensures that services remain focused on end-of-life care. While some studies have explored how providers might adjust admissions and discharges in response to this cap, the overall impact on costs has been found to be modest. For more on how payment incentives affect providers, check out this Study on provider payment incentives.
Understanding these limits is part of navigating Medicare Costs effectively.
What are the patient’s out-of-pocket costs?
One of the most reassuring aspects of the Medicare hospice benefit is how minimal the patient’s out-of-pocket costs are. Medicare covers nearly all the costs related to the terminal illness once you elect hospice.
- No Deductible: Unlike many other Medicare services, there is no deductible for hospice care.
- Part A and B Premiums: You will continue to pay your monthly Medicare Part A (if applicable) and Part B premiums. These premiums cover services unrelated to your terminal illness.
- Coinsurance for Respite Care: For inpatient respite care, you may have a small coinsurance. This is 5% of the Medicare-approved amount for the respite stay. For example, if Medicare approves a daily rate of around $519 for respite, your coinsurance would be about $26 per day. This amount is capped by the annual Part A inpatient hospital deductible.
- Copayment for Prescription Drugs: You may have a copayment of up to $5 per prescription for outpatient prescription drugs used for pain and symptom management related to your terminal illness.
For all other services, supplies, and equipment related to your terminal illness, Medicare covers 100% of the cost. This financial relief allows patients and families to focus on comfort and support during a challenging time.
How does hospice work with a Medicare Advantage Plan?
This is a crucial point that often causes confusion. Even if you are enrolled in a Medicare Advantage Plan (like an HMO or PPO), hospice care is covered by Original Medicare (Part A), not your Medicare Advantage Plan.
This means:
- Original Medicare Carve-Out: When you elect the hospice benefit, your hospice care is “carved out” from your Medicare Advantage Plan. Original Medicare becomes responsible for paying for all services related to your terminal illness.
- Maintaining MA Benefits: You remain enrolled in your Medicare Advantage Plan and continue to receive all your other Medicare benefits (for conditions unrelated to your terminal illness) through that plan.
- Coordination: Your hospice team will coordinate with your Medicare Advantage Plan to ensure all care, whether related or unrelated to your terminal illness, is properly managed and covered.
This structure ensures that everyone eligible for Medicare hospice benefits receives the same comprehensive coverage, regardless of their chosen Medicare plan.
Frequently Asked Questions about Medicare Hospice Payments
We often hear common questions about the practicalities of Medicare hospice coverage. Let’s address some of these to provide even greater clarity.
How long will Medicare pay for hospice care?
Medicare will pay for hospice care as long as you continue to meet the eligibility requirements. The initial eligibility requires a doctor and a hospice doctor to certify that you are terminally ill and have a prognosis of 6 months or less if your illness runs its normal course.
Hospice care is provided in specific benefit periods:
- Two 90-day periods: These are the initial periods of coverage.
- Unlimited 60-day periods: After the initial 90-day periods, you can have an unlimited number of 60-day periods.
Before each new benefit period (after the first 90-day period), the hospice medical director or another hospice doctor must recertify that you are still terminally ill. This ensures that you continue to meet the eligibility criteria for the benefit. As long as you meet these requirements, Medicare will continue to pay for your hospice care.
Can I stop hospice care at any time?
Absolutely! Choosing hospice care is a voluntary decision, and you have the right to change your mind at any point. If you decide that hospice care is no longer right for you, or if you wish to pursue curative treatments again, you can stop the hospice benefit.
To do this, you simply need to sign a form that revokes your hospice election. Once you do, you will return to your Original Medicare coverage (or your Medicare Advantage Plan) for all your healthcare needs. You can also re-elect hospice care at a later time if you become eligible again and wish to resume the benefit. It’s all about ensuring your care aligns with your wishes and needs.
What isn’t covered by the Medicare hospice benefit?
While the Medicare hospice benefit is incredibly comprehensive for services related to your terminal illness, there are a few things it generally won’t cover:
- Treatments to cure the terminal illness: The core philosophy of hospice is palliative care (comfort and symptom management), not curative treatments. If you choose hospice, you agree to forgo treatments aimed at curing your terminal illness.
- Prescription drugs unrelated to the terminal illness: While hospice covers drugs for pain and symptom management related to your terminal illness, medications for conditions unrelated to your terminal diagnosis (e.g., blood pressure medication for a stable, chronic condition) would typically be covered under your Medicare Part D plan or other insurance.
- Room and board in a facility (unless for GIC/IRC): Medicare hospice generally does not cover the cost of room and board if you live in a nursing home, assisted living facility, or hospice inpatient facility. The exceptions are for short-term General Inpatient Care (GIC) or Inpatient Respite Care (IRC), which are covered because they are for acute symptom management or caregiver relief, not permanent residence.
- Care from providers not arranged by the hospice team: All services for your terminal illness must be provided or arranged by your chosen hospice team. If you receive care from an outside provider for your terminal illness without your hospice team’s arrangement, Medicare may not cover it, and you could be responsible for the full cost.
It’s always best to communicate openly with your hospice team about any care or services you think you might need to ensure they are covered and properly coordinated.
Conclusion
Understanding how much Medicare pays hospice per day reveals a structured and comprehensive system designed to provide comfort and support during a terminal illness. Medicare’s per-diem payment model, with its four distinct levels of care—Routine Home Care, Continuous Home Care, General Inpatient Care, and Inpatient Respite Care—ensures that providers are reimbursed for a wide range of services. From the standard daily rates for routine home care, adjusted for the length of stay, to the higher rates for crisis management and inpatient support, the system aims to align payments with patient needs.
We’ve explored how Medicare covers nearly all costs related to the terminal illness, with minimal out-of-pocket expenses for beneficiaries, and how hospice care is a carve-out benefit under Original Medicare, even if you have a Medicare Advantage Plan. This comprehensive coverage allows individuals and their families to focus on quality of life and emotional well-being rather than financial burdens.
Planning for retirement, including understanding healthcare benefits like Medicare hospice, is crucial. We Can Help You, Inc. is dedicated to educating individuals on Medicare and Social Security, empowering you to make informed decisions for a secure future. For a complete guide on navigating these benefits, explore our resources on Navigating Medicare and Hospice Care: Understanding Costs and Coverage.